Human Blood Cells Types Showing Red Blood Cells, White Blood Cells, Platelets, and Their Function in the Human Circulatory System
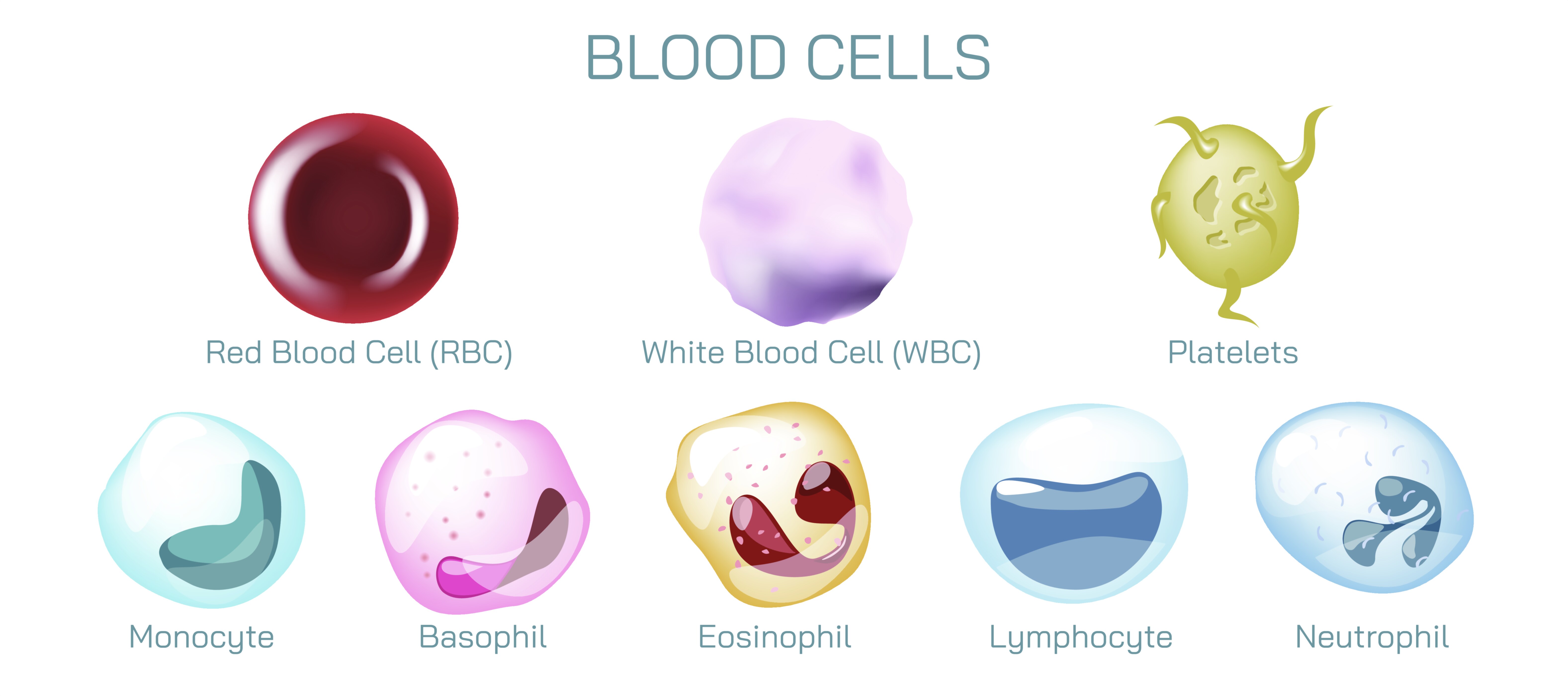
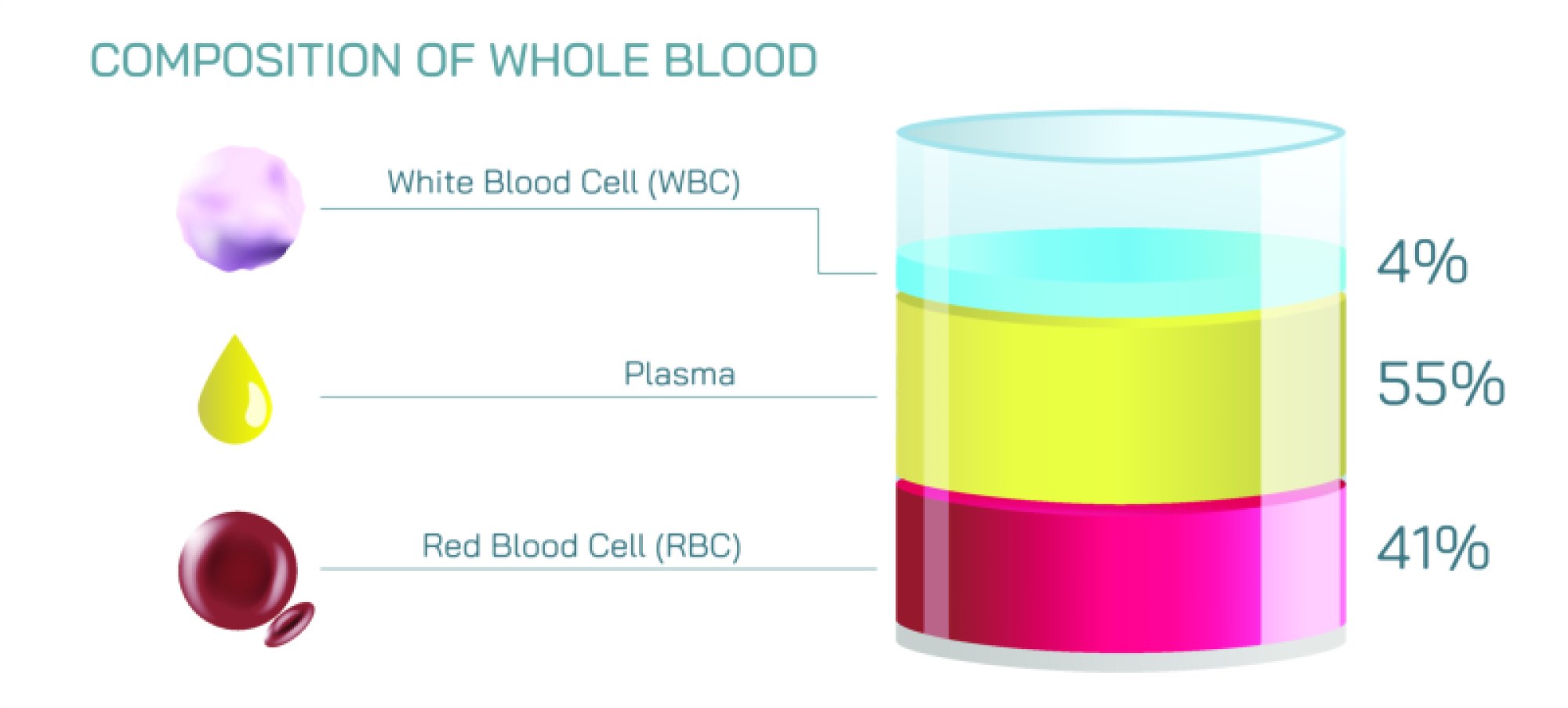
Blood is not a single uniform fluid, but a living transport medium composed of specialized cells suspended in plasma, each designed to perform a particular function essential for survival. A vector illustration showing the different types of human blood cells usually highlights three major cellular components — red blood cells, white blood cells, and platelets — revealing how each of them contributes to circulation, immunity, oxygen delivery, healing, and tissue preservation. Although these cells flow side by side within the same vascular system, they differ greatly in structure, life span, and physiological purpose. Taken together, they form a remarkably coordinated cellular network that keeps the body nourished, protected, and repaired every second of life.
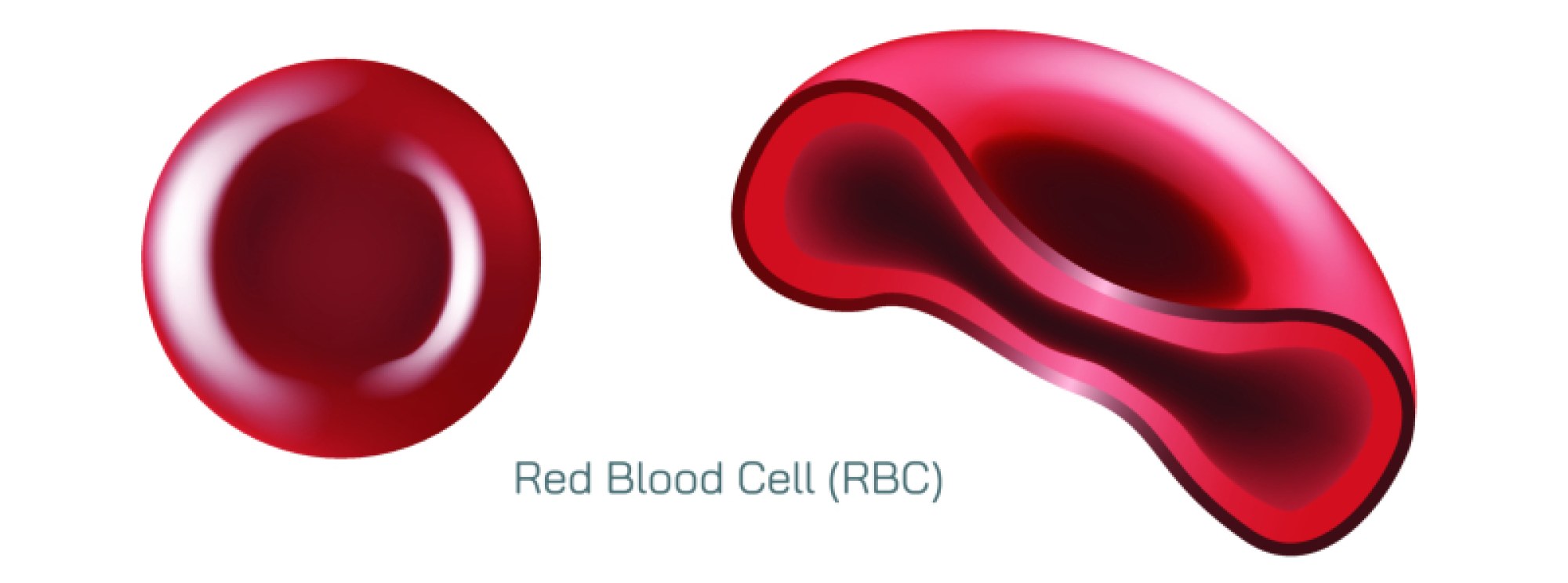
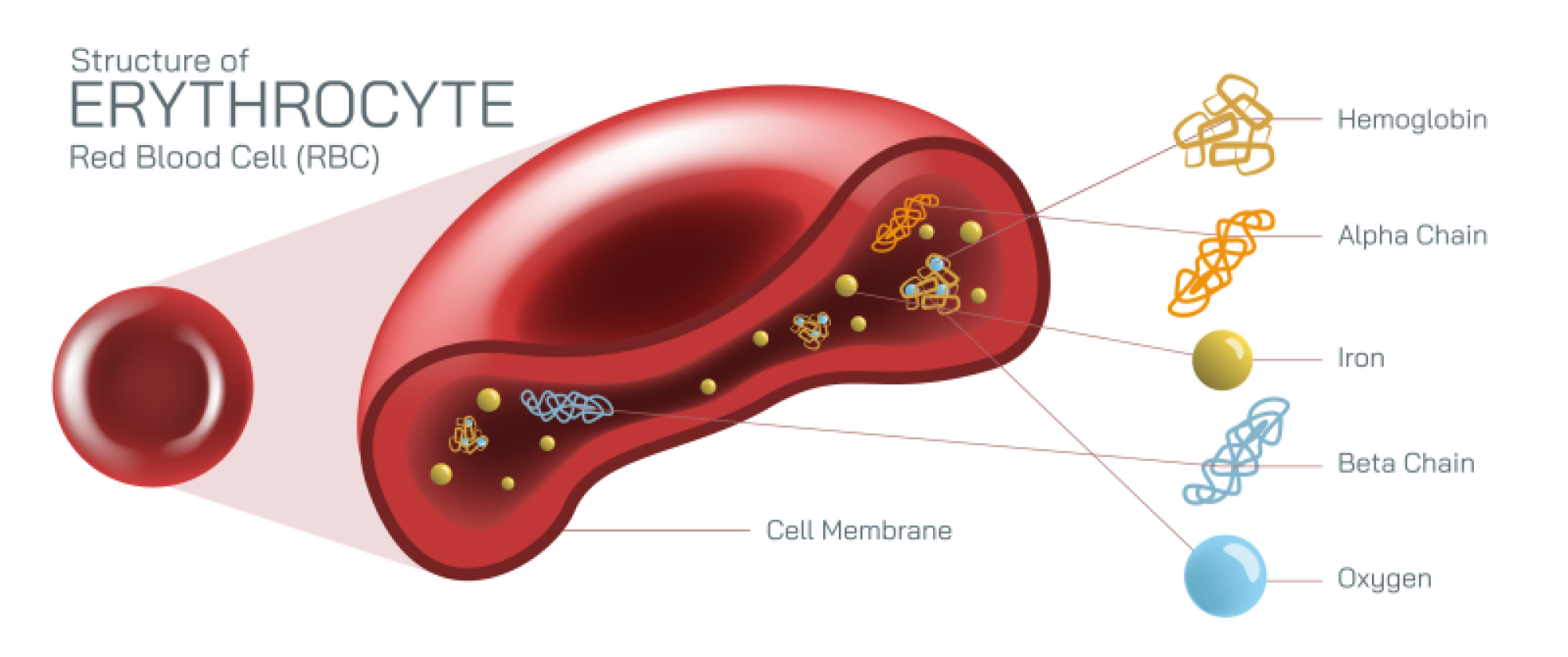
Red blood cells — also known as erythrocytes — make up the majority of circulating blood cells and are visually distinctive in illustrations due to their round, biconcave disc shape. This inward-curved structure is not accidental; it dramatically increases the cell’s surface area and flexibility, enabling efficient gas exchange and smooth passage through capillaries thinner than the cells themselves. Red blood cells carry hemoglobin, an iron-rich protein that binds oxygen in the lungs and transports it to tissues throughout the body, then collects carbon dioxide and returns it to the lungs to be expelled. Their lack of a nucleus allows more space for hemoglobin but also means they cannot divide or repair themselves, giving them a finite lifespan of roughly 120 days. The enormous number of red blood cells and the constant cycle of renewal reflect the body’s high demand for oxygen transport — without adequate red cells or hemoglobin, tissues starve for oxygen, leading to fatigue, weakness, and potentially life-threatening complications.
While red blood cells focus on oxygen transport, white blood cells — or leukocytes — defend the body against infection and foreign intruders. They are far fewer in number than red cells, but their role is pivotal: they detect, target, and neutralize microbes, viruses, toxins, and abnormal self-cells. In a vector illustration, white blood cells are often shown larger and more irregularly shaped than red cells, reflecting both their size and adaptability. Unlike red blood cells, white blood cells contain nuclei and complex internal structures, enabling them to move independently, change shape, and coordinate immune responses. This category includes diverse subtypes — such as neutrophils that attack bacteria, lymphocytes that produce antibodies and store immune memory, and macrophages that engulf pathogens and cellular debris. White blood cells patrol the bloodstream and tissues continuously, increasing rapidly during infection or inflammation. Their ability to recognize antigens and orchestrate the broader immune defense makes them essential guardians of the circulatory and lymphatic systems.
The third major cellular component of blood, platelets — or thrombocytes — play a crucial role in preventing blood loss and repairing damaged vessels. Though much smaller than red or white cells, platelets act as the frontline responders in wound healing. When a blood vessel is injured, platelets rush to the site, become activated, and clump together to form an initial platelet plug. They then trigger a complex cascade that solidifies this plug into a blood clot by converting circulating fibrinogen into fibrin, forming a stabilizing mesh. In illustrations, platelets are usually shown as tiny fragments rather than fully shaped cells because they originate from the cytoplasm of larger bone marrow cells called megakaryocytes and lack nuclei. While clotting is normally protective, platelets must be tightly regulated — excessive clotting can block vessels and lead to strokes or heart attacks, while insufficient platelet function allows uncontrolled bleeding. Their ability to strike this balance demonstrates the precision of hematological regulation within the circulatory system.
Together, red blood cells, white blood cells, and platelets form the cellular foundation of the human circulatory system, each performing a separate but interdependent duty that sustains life. Red cells supply the body with oxygen and clear carbon dioxide, ensuring that energy metabolism continues in every organ and tissue. White cells operate as the immune surveillance network, constantly scanning for threats and activating defense strategies with molecular accuracy. Platelets preserve vascular integrity by responding instantly to injury, sealing broken vessels and initiating repair. These differences in function explain the importance of maintaining proper blood composition; a deficiency or malfunction in any category produces serious systemic consequences. Anemia reduces oxygen availability, immune disorders increase vulnerability to infection, and clotting disorders threaten survival during injury or surgery.
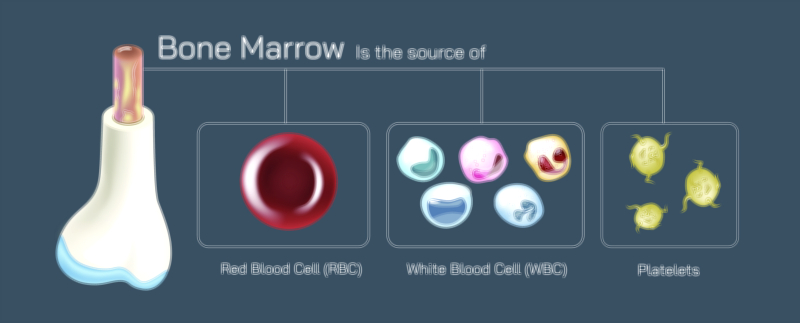
The diverse functions of these cells reflect their equally diverse origins and life cycles. All three arise in the bone marrow from hematopoietic stem cells, which differentiate into specialized blood cell lines. Red blood cells are produced in high numbers due to constant demand for oxygen transport, while production of white cells rises sharply during infection or immune challenge. Platelets are generated in bursts as megakaryocytes extend cytoplasmic filaments that fragment into thousands of tiny platelet particles. Once released into circulation, red blood cells circulate for months, platelets for about a week, and some white cells for mere hours or days — though memory white cells formed during immune priming can persist for years. This dynamic turnover ensures that the blood maintains balance despite wear, breakdown, and physiological stress.
Blood cells do not operate in isolation — their cooperation illustrates the circulatory system’s ability to maintain homeostasis. During intense physical activity, red blood cells deliver extra oxygen to muscles while platelets stand ready in case of micro-tears in tissues. During infection, white blood cells migrate to affected areas while clotting mechanisms prevent damage from inflamed or weakened vessels. During illness or nutrient deficiency, the appearance of blood cells often changes, becoming a valuable diagnostic window. Red cells may shrink or become pale during iron deficiency; white cells spike during infection; platelets fluctuate during autoimmune or bone marrow disorders. This is why blood tests are an essential medical tool — they provide a real-time reflection of the body’s internal condition by measuring and analyzing these populations.
A vector illustration of blood cell types often arranges the three categories together in a balanced scene: plentiful biconcave red blood cells flowing smoothly through a vessel, a few enlarged and irregular white cells demonstrating immune surveillance, and tiny platelets shown as scattered fragments ready for activation. Even without narrative text, the viewer can interpret the message — different cells, different structures, different jobs — all contributing to the same vital system. When understood collectively, red blood cells represent energy availability, white blood cells represent protection, and platelets represent repair.
The human circulatory system functions successfully because of this cellular teamwork. Oxygen delivered today supports the muscles that move the body; immune defense prevents microscopic threats from taking hold; and clotting ensures that even daily minor injuries heal without harm. Through their constant movement and specialization, red blood cells, white blood cells, and platelets allow life to continue moment by moment. In one unified flow of plasma, the body transports fuel, eliminates waste, protects itself, and rebuilds where damage has occurred. The vector illustration showing these cell types does more than represent anatomy — it captures the quiet but powerful cellular engine that sustains the continuity of human life.