Diabetes Type One and Type Two Showing Glucose Regulation, Insulin Activity, and Pancreatic Function Difference
Diabetes is fundamentally a disorder of glucose regulation, and although both Type 1 and Type 2 diabetes result in elevated blood sugar levels, the underlying mechanisms differ dramatically. A vector illustration comparing these two forms of diabetes typically shows the flow of glucose in the bloodstream, the role of the pancreas in insulin production, and how insulin activity affects cellular uptake of glucose. By visually contrasting how glucose behaves in a healthy body versus in Type 1 and Type 2 diabetes, the illustration captures how the same biological system can fail in different ways, leading to similar outward symptoms but distinct causes and treatment needs.
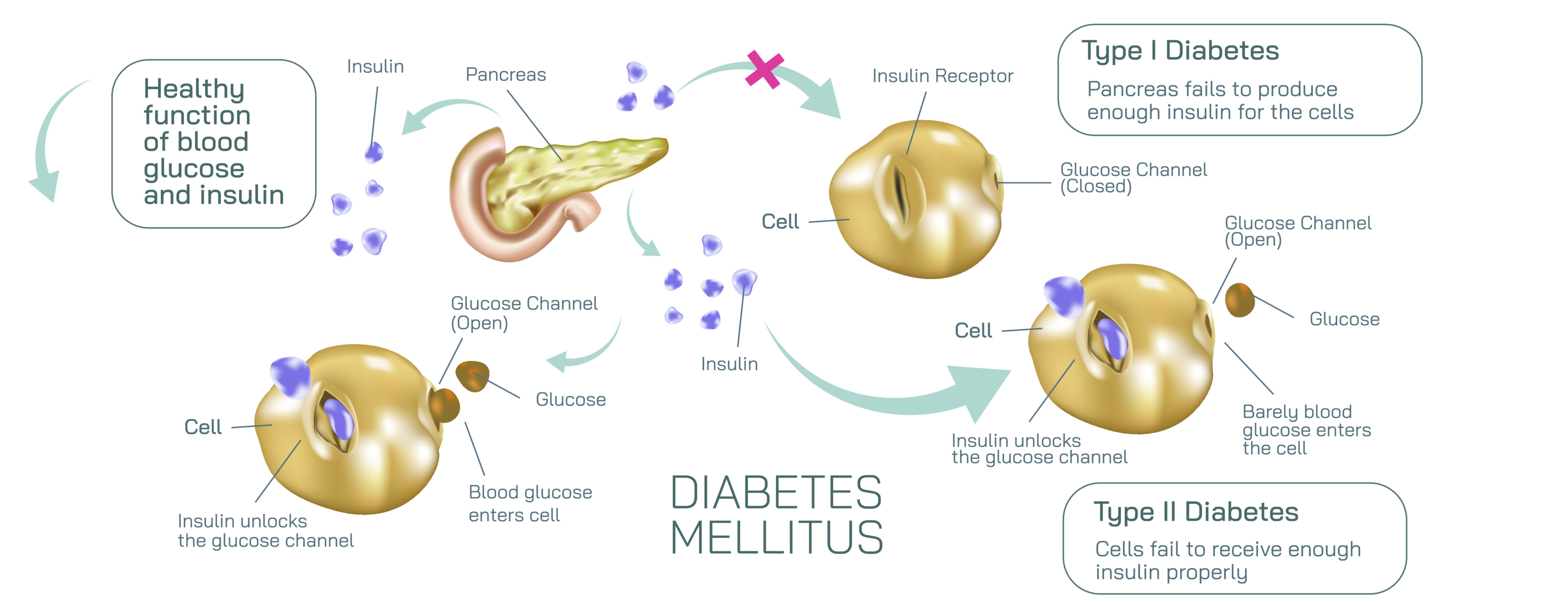
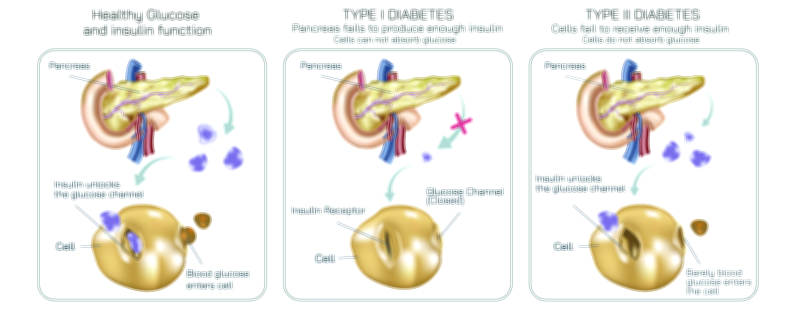
In a healthy body, blood glucose rises after meals as food is broken down and sugars enter the bloodstream. The pancreas, specifically the beta cells in the islets of Langerhans, continuously monitors glucose levels and releases insulin when levels increase. Insulin acts like a biochemical “key” that unlocks body cells — muscle, fat, and liver — enabling glucose to enter and be used as energy. With insulin present and functioning correctly, blood sugar returns to normal and cells stay nourished. This flowing cycle of glucose entry, insulin release, and cell uptake is typically illustrated with smooth arrows showing stable glucose regulation.
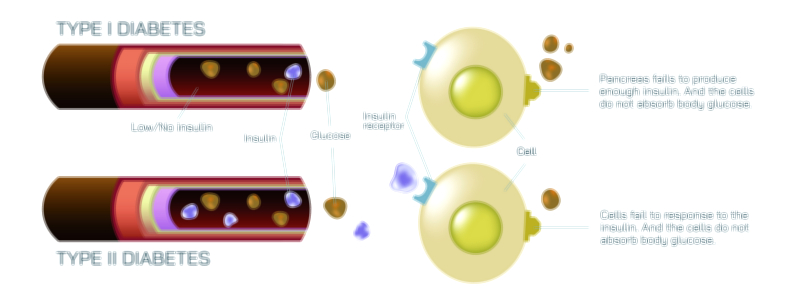
Type 1 diabetes dramatically disrupts this process at its starting point: insulin is nearly absent. The pancreas loses its ability to produce insulin because the immune system mistakenly destroys the beta cells responsible for making it. In a vector illustration, this distinction becomes clear: the pancreas is shown releasing little or no insulin, and arrows representing glucose movement remain stuck in the bloodstream because cells cannot open without the insulin “key.” Even though glucose is plentiful, cells cannot access it, leading to dangerously high blood sugar levels and a lack of energy inside cells. This is why individuals with Type 1 diabetes require external insulin for survival — their bodies cannot make it internally. Illustrations often represent this dependency by including icons of insulin injections or pumps beside the Type 1 model.
Type 2 diabetes, on the other hand, is rooted in insulin resistance — insulin is present, but cells do not respond to it properly. In an illustration, the pancreas can be shown releasing insulin in normal or even above-normal amounts, but arrows indicating glucose entry into cells appear blocked, reflected, or obstructed. The insulin does attempt to unlock the cells, but the cell receptors act as if they cannot “hear” the insulin signal. Because glucose cannot enter easily, the body experiences high blood sugar even though insulin exists. Over time, the pancreas becomes overworked and may reduce its production of insulin, creating a dual problem: insulin resistance plus declining insulin release. Type 2 diabetes often develops slowly, and the body spends years trying to compensate before blood sugar remains chronically high.
Both types of diabetes share the same outcome — consistently elevated blood glucose in the bloodstream — but for different biological reasons. That difference drives the distinct treatment approaches. For Type 1 diabetes, the pancreas cannot produce insulin, so the essential solution is insulin replacement from external sources. For Type 2 diabetes, the focus centers on improving cellular sensitivity to insulin, reducing glucose production in the liver, and balancing diet and physical activity. If the pancreas eventually becomes too fatigued to meet the demands of insulin resistance, external insulin may also become necessary.
A vector illustration makes these differences visually intuitive by showing how glucose moves — or fails to move — from the bloodstream into the cells under each condition. Typical diagram elements include:
• A healthy model, showing insulin effectively transporting glucose into cells.
• A Type 1 model, showing little to no insulin release from the pancreas and glucose remaining outside cells.
• A Type 2 model, showing insulin release present but impaired cellular uptake due to insulin resistance.
• Clear arrows showing whether glucose enters the cells (healthy), remains trapped (Type 1), or is partially resisted (Type 2).
• Blood sugar levels shown rising above normal in both types because glucose continues to accumulate in the bloodstream.
What makes these illustrations powerful is not just the accuracy of the comparison but the clarity they bring to the lived experience of diabetes. For a person with Type 1 diabetes, the challenge revolves around replacing the missing insulin and matching doses to food, physical activity, and metabolism throughout the day. For a person with Type 2 diabetes, the challenge revolves around restoring the cells’ ability to respond to insulin and preventing long-term exhaustion of the pancreas. Both conditions require mindful management because prolonged elevation of blood glucose can harm blood vessels, nerves, kidneys, eyes, and the heart.
Yet beneath the clinical dimension is an elegant biological truth: every cell in the body depends on glucose for survival, and insulin is the mediator that controls access to it. If insulin is not present (Type 1) or not effective (Type 2), the body remains full of energy it cannot use. This paradox — energy-starved cells inside a bloodstream rich with sugar — lies at the heart of diabetes. By highlighting insulin absence versus insulin resistance and showing how the pancreas differs in each case, the illustration transforms an abstract medical concept into a visually clear explanation of how diabetes disrupts the body’s normal energy cycle.
Through the lens of glucose flow, insulin action, and pancreatic function, the comparison of Type 1 and Type 2 diabetes becomes not only scientifically precise but deeply intuitive. A single vector illustration has the power to tell the complete story: how the body regulates blood sugar when the system works, how the regulation collapses in each type of diabetes, and why both forms require lifelong care to restore balance in the most vital biological process — the use of glucose as fuel for life.