Types of Blood Groups and Their Classification – Understanding ABO and Rh Systems, Antigen–Antibody Interactions, Genetic Inheritance, Universal Donors and Recipients, and the Crucial Role of Blood Group Compatibility in Medicine and Human Biology
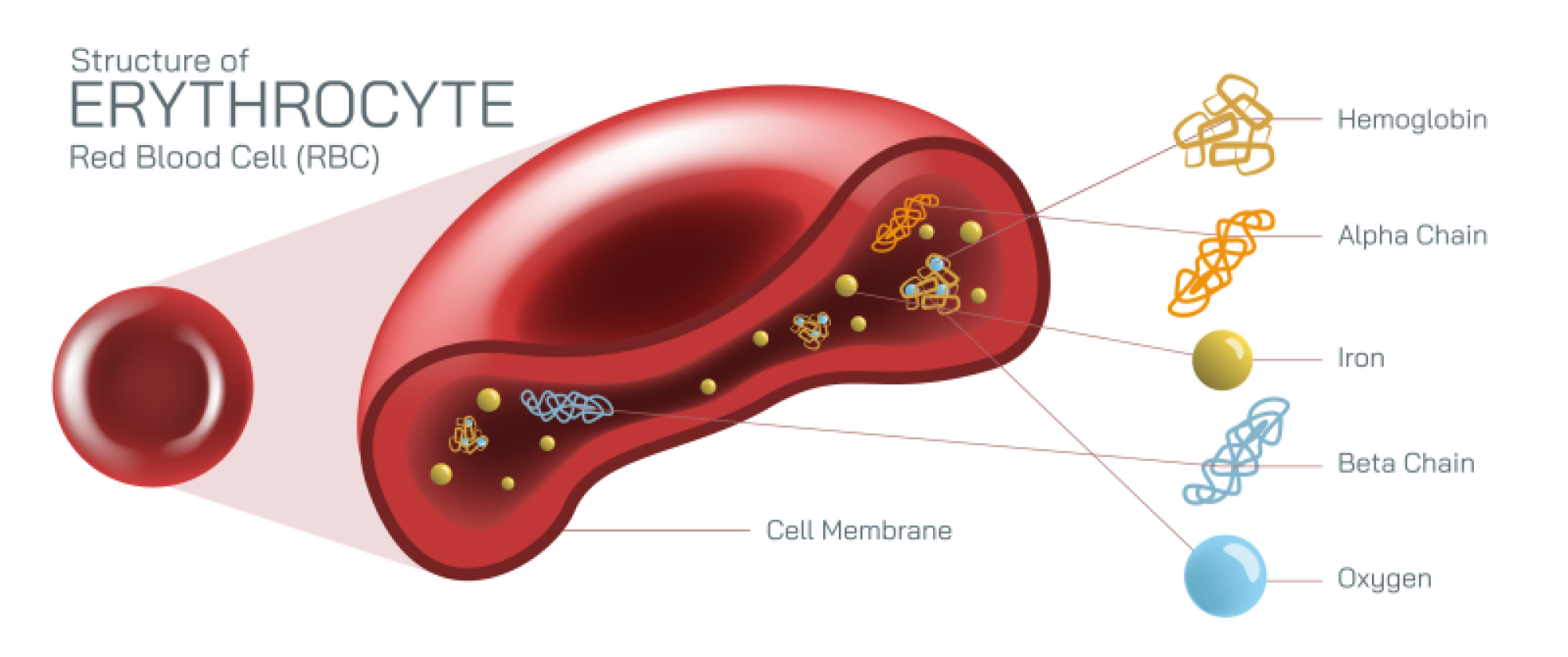
Blood groups form one of the most vital biological classifications in human physiology because they determine how the immune system reacts to transfusions, organ transplants, pregnancy, and even certain medical conditions. Although at first glance blood may appear uniform in every human being, microscopic differences in the molecules present on the surface of red blood cells create categories that are biologically distinct. These surface molecules, known as antigens, are inherited genetically and act like identity markers that allow the immune system to recognize what belongs to the body and what does not. When blood that does not match a person’s antigen profile enters their circulation, the immune system may launch a strong defensive attack in the form of an agglutination or clotting reaction that can be fatal. For this reason, the classification of blood groups is not only a scientific matter but also an essential component of medical safety in transfusions, surgeries, childbirth, and emergency care. Understanding the different types of blood groups reveals how genetics, immunity, and medicine intersect to protect human health.
The ABO Blood Group System – The Primary Classification Based on Antigens and Natural Antibodies
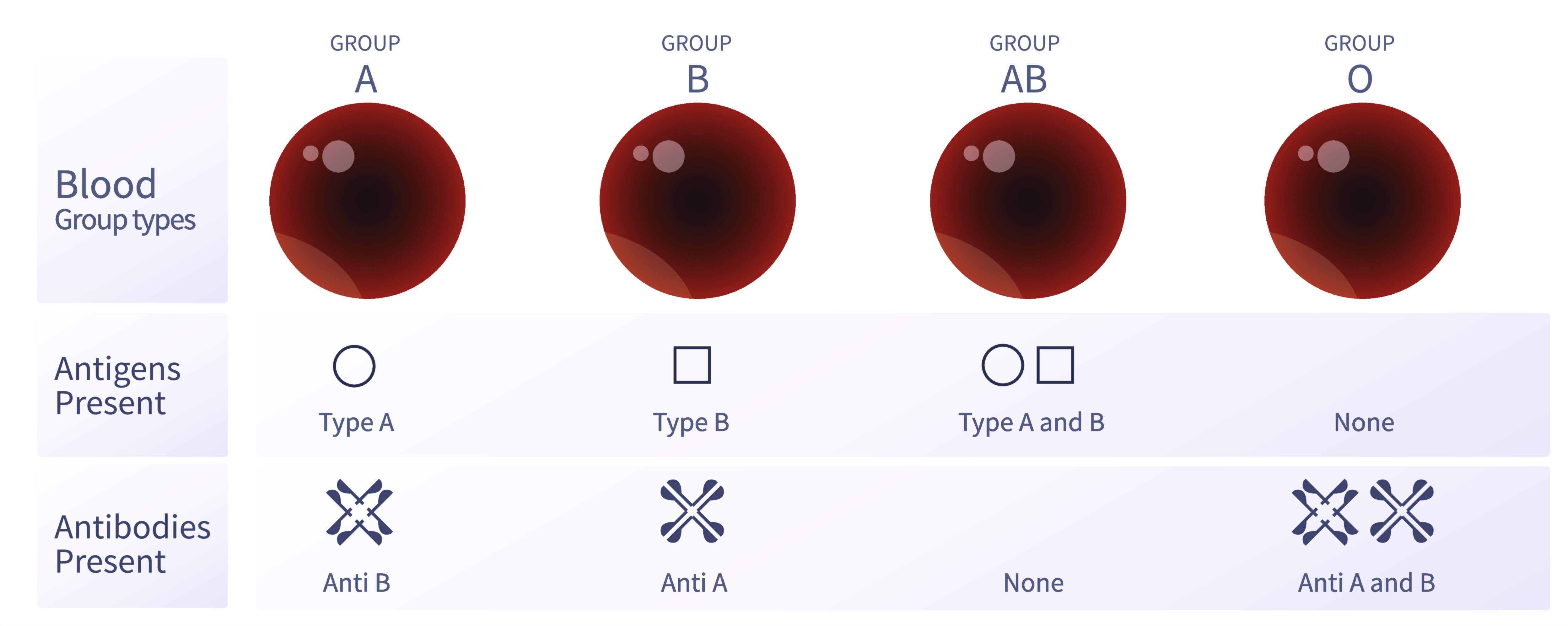
The most widely recognized and clinically significant system of blood classification is the ABO blood group system. This system categorizes blood according to the presence or absence of two main antigens—A and B—located on the surface of red blood cells. If an individual has the A antigen, they belong to group A; if they have the B antigen, they belong to group B; if they possess both A and B antigens, they belong to group AB; and if neither antigen is present, they belong to group O. This classification is essential because the immune system naturally contains antibodies against whichever antigens are not present on its own red blood cells. For example, a person with group A blood has anti-B antibodies, a person with group B blood has anti-A antibodies, a person with group O blood has both anti-A and anti-B antibodies, and a person with AB blood has neither type of antibody. This antigen–antibody balance determines which blood types can safely mix and which will trigger an immune reaction.
Group O stands out because individuals with this blood type lack both antigens and therefore produce both anti-A and anti-B antibodies. As a result, the red blood cells of group O can be safely given to recipients of any ABO type, earning it the title “universal donor” for red cell transfusions. In contrast, group AB individuals have both antigens and no antibodies, allowing them to receive blood from any ABO group but donate only to AB recipients, making them the “universal recipient.” This compatibility rule exemplifies the precision with which the body identifies what does and does not belong in the bloodstream. These interactions explain why a mistake in ABO matching during a transfusion can cause rapid clumping and destruction of red blood cells, leading to shock, kidney failure, and potentially death. Thus, the ABO system is the first and most critical safeguard in transfusion medicine.
The Rh Blood Group System – Understanding Positive and Negative Status
The second major pillar of blood classification is the Rh (Rhesus) system, which is most commonly referenced in the form of the Rh factor. This classification depends on the presence or absence of the D antigen on the red blood cell surface. If the D antigen is present, the person is Rh-positive; if it is absent, the person is Rh-negative. These two states do not change the ABO category but modify it by adding a positive or negative suffix. Thus, eight common ABO–Rh combinations exist: A+, A–, B+, B–, AB+, AB–, O+, and O–. Rh compatibility becomes particularly important because an Rh-negative individual does not naturally carry anti-D antibodies, but will produce them if exposed to Rh-positive blood. While this immune response poses risks in transfusion, its most dramatic medical relevance appears in pregnancy.
When an Rh-negative mother carries an Rh-positive fetus—often inherited from an Rh-positive father—the mother’s immune system may produce anti-D antibodies if fetal blood mixes with hers during childbirth, miscarriage, or certain medical procedures. In subsequent pregnancies with another Rh-positive fetus, those antibodies can cross the placenta and attack fetal red blood cells, resulting in hemolytic disease of the newborn, a severe and sometimes fatal condition. Modern medicine prevents this complication by administering Rh immunoglobulin injections to Rh-negative mothers to block antibody formation. The Rh system therefore shows how understanding blood group classification is not only vital for transfusions but also essential for maternal and pediatric health.
ABO and Rh Systems Together – The Basis for Safe Transfusion Practices
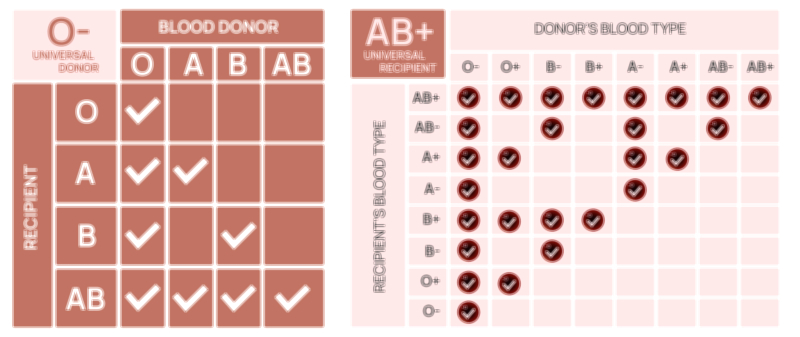
In medical practice, safe blood transfusion depends on matching both the ABO and Rh classifications. While it is often assumed that transfusion simply requires finding blood of the same type, the compatibility network is more precise. For example, O– blood is the true universal donor for red cells because it lacks A, B, and Rh antigens, reducing the risk of immune reactions even in emergencies when matching time is limited. In contrast, AB+ individuals are the universal recipients for red cells because they do not possess antibodies against any major blood group antigen. However, the compatibility matrix changes depending on whether the transfused blood component is whole blood, red cells, plasma, or platelets, because the antibody content and antigen distribution vary among blood components. This complexity highlights the need for meticulous medical screening, cross-matching tests, and computerized blood-bank cataloging to prevent patient harm.
Inheritance of Blood Groups – The Genetic Perspective Behind Classification
The inheritance of blood groups follows predictable patterns of Mendelian genetics. The genes determining ABO blood type reside on chromosome 9 and are inherited in pairs—one from each parent. The A and B alleles are codominant, meaning that if both are inherited (A from one parent and B from the other), both antigens appear, producing AB blood type. The O allele is recessive, which means an individual has type O only when both alleles are O. In the Rh system, the positive allele is dominant over the negative, meaning that a person needs only one positive allele to be Rh-positive. These genetic patterns explain why blood types are familial yet not always predictable at first glance. Understanding inheritance has implications not only for biology education but also for forensic science, paternity investigations, and anthropological research tracing human migration and ancestry.
Global Distribution and Medical Significance of Blood Groups
Blood group distribution varies greatly around the world. For instance, O+ is the most common type globally, especially in Latin America and parts of Africa, while A and B vary widely across Europe and Asia. AB remains the rarest worldwide. These distribution patterns are not random; they reflect historical evolutionary pressures, diseases, and population migrations. For example, some research shows that certain blood groups offer partial protection or increased susceptibility to infections such as cholera, malaria, and influenza. Therefore, blood group classification carries both immunological and evolutionary relevance and continues to be a subject of global biomedical study.
Beyond ABO and Rh – Extended Blood Group Systems
Although ABO and Rh are the most clinically dominant systems, more than forty additional blood group systems exist, including Kell, Duffy, Kidd, MNS, and Lewis. These systems become especially important in patients who receive repeated transfusions, such as those with sickle-cell disease, thalassemia, or chronic anemia, because the body may eventually react to minor antigens. Sophisticated medical screening ensures that transfusion-dependent patients receive extended antigen matching to prevent long-term complications, further showing why blood classification is a dynamic and evolving field.
Ultimately, the classification of blood groups is not an abstract scientific category but a life-preserving system deeply rooted in genetics, immunity, and medical practice. Every labeled blood bag, cross-matching test, and prenatal screening depends on the precise identification of ABO and Rh types to protect patients against immune reactions. Blood groups teach us that even within the shared biology of humanity, microscopic molecular differences determine whether transfusion heals or harms. By understanding the types of blood groups and their classification, learners gain a deeper appreciation of how human biology safeguards itself and how medicine uses this knowledge to save lives every single day.