Chronic Liver Disease — Progressive Liver Damage, Metabolic Dysfunction, Organ Failure Risk, and Long-Term Impact on Human Health
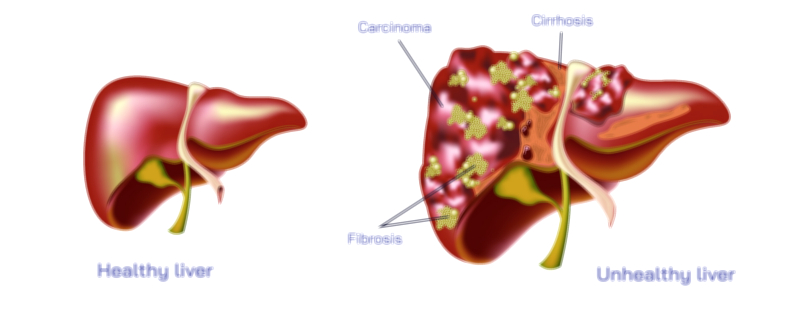
Chronic liver disease refers to a long-lasting and progressive deterioration of liver structure and function that develops over months or years rather than appearing suddenly. The liver is one of the most vital organs in the human body, responsible for detoxifying blood, regulating metabolism, producing bile for digestion, synthesizing clotting factors, storing nutrients, and supporting immune function. When damage becomes persistent, the liver begins to lose its ability to repair and regenerate effectively. Instead of healing with healthy tissue, the organ gradually develops scarring known as fibrosis. With time, fibrosis may advance to cirrhosis, where the normal tissue is replaced almost entirely by hardened scar tissue, severely restricting blood flow through the liver and interfering with its functions. Chronic liver disease is therefore not a single illness but a spectrum of pathological changes that lead toward progressive liver failure. The disorder develops silently in many individuals, and symptoms may not appear until significant injury has already taken place, making early detection and management essential for long-term health outcomes.
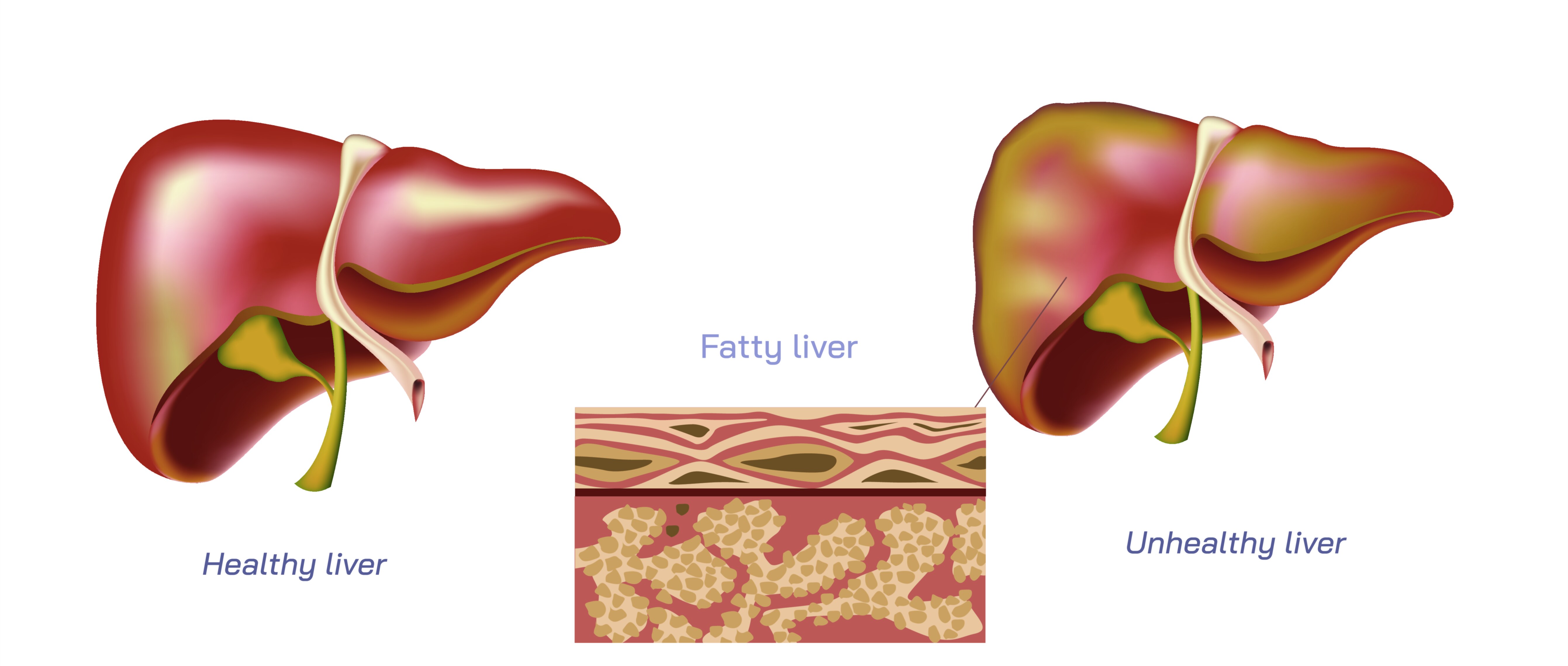
The development of chronic liver disease is driven by continuous injury from a variety of causes, including excessive alcohol intake, viral infections such as hepatitis B and hepatitis C, metabolic dysfunction-associated steatotic liver disease (formerly fatty liver disease), autoimmune disorders, congenital metabolic abnormalities, prolonged drug toxicity, and exposure to environmental toxins. One of the most common modern causes is fat accumulation in liver cells associated with metabolic disorders, obesity, sedentary lifestyle and insulin resistance. Alcohol-related liver disease, another major contributor, results from toxic effects of repeated heavy drinking that trigger inflammation and fat deposition. Viral hepatitis remains a significant cause in many countries, where chronic infection leads to sustained inflammation that gradually destroys liver cells. Autoimmune hepatitis causes the immune system to mistake liver cells for harmful invaders, creating persistent inflammation that leads to scarring. In all of these pathways, the unifying theme is repeated injury and incomplete healing, which slowly converts a healthy liver into a structurally distorted and functionally impaired organ.
During the initial stages of chronic liver disease, the body often compensates for reduced liver function, leading many individuals to be unaware of the process taking place. Early fibrosis produces no obvious symptoms, and the liver can continue functioning even when partially damaged. Over time, however, the accumulation of scar tissue disrupts blood circulation within the liver, increasing internal pressure in the portal venous system and interfering with the processing of nutrients, hormones, drugs and toxins. People may begin to notice fatigue, weakness, abdominal discomfort, loss of appetite, nausea, unexplained weight loss or gain, and yellowing of the skin and eyes caused by jaundice. As liver function continues to decline, other complications emerge: swelling of the legs and abdomen due to fluid buildup, bleeding problems caused by reduced clotting factor production, mental confusion due to accumulation of toxins in the brain, and increased susceptibility to infections. When cirrhosis becomes severe, the liver can no longer compensate, leading to irreversible organ failure and the need for transplantation.
The progression of chronic liver disease reflects a dynamic and sometimes reversible process. In early stages, when inflammation and mild scarring are present, lifestyle modification, removal of the underlying cause, and medical treatment may allow the liver to regenerate and partially reverse damage. For example, complete alcohol abstinence can dramatically reduce long-term injury in people with early alcohol-related liver disease, and antiviral treatment for hepatitis C can stop viral replication and allow fibrotic tissue to remodel. Effective treatment of metabolic dysfunction through weight loss, dietary modifications, glucose control and exercise can reduce fat buildup and inflammation in the liver. In autoimmune liver disease, immunosuppressive therapies can protect the organ from immune-mediated destruction. These improvements highlight the liver’s extraordinary ability to repair itself when harmful conditions are removed early enough. However, once cirrhosis becomes established and scar tissue has replaced most of the liver’s functional cells, the damage becomes largely permanent, and treatment focuses on slowing further progression and managing complications.
Complications represent some of the most dangerous consequences of chronic liver disease. Portal hypertension occurs when scar tissue blocks normal blood flow through the liver, forcing blood to reroute through fragile veins that may swell and rupture, especially in the esophagus and stomach. Ascites, the buildup of fluid in the abdomen, develops when pressure changes in blood vessels combine with reduced protein production in the liver. Hepatic encephalopathy arises when toxins such as ammonia accumulate in the bloodstream and reach the brain, causing confusion, personality changes, disorientation, and in severe cases, coma. People with cirrhosis also have a much higher risk of hepatocellular carcinoma, a primary liver cancer that often develops silently and progresses quickly. These complications highlight how chronic liver disease affects not only the organ itself but also the entire body through metabolic, circulatory and neurological pathways.
Diagnosis of chronic liver disease typically requires a combination of medical history, physical examination, blood tests, imaging studies and sometimes biopsy. Blood tests may reveal abnormal liver enzyme levels, reduced albumin production, impaired clotting ability, or markers of viral infections. Imaging techniques such as ultrasound, CT scan or MRI can detect fat buildup, fibrosis, nodules or irregular texture. Specialized tools such as elastography measure liver stiffness to assess fibrosis without invasive procedures. In certain cases, a liver biopsy remains the most direct method to determine the severity and cause of liver injury. Early diagnosis is particularly important because interventions are most effective before severe scarring develops.
Treatment depends on the underlying cause and stage of the disease. Eliminating damaging triggers—such as alcohol, hepatitis infection or untreated metabolic disease—is the first step. Medications may be used to manage inflammation, control viral infection, regulate the immune system or relieve symptoms. Clinical care focuses on minimizing complications with strategies such as diuretics for ascites, blood pressure medications to reduce portal hypertension, lactulose for encephalopathy, and nutritional therapy to prevent muscle wasting. Advanced cirrhosis eventually requires evaluation for liver transplantation, which remains the only definitive treatment when irreversible organ failure occurs. Transplantation replaces the damaged liver with a healthy donor organ, restoring metabolic function and dramatically improving survival in eligible patients.
Although chronic liver disease is a serious and potentially life-threatening condition, prevention and early intervention play critical roles in improving long-term outcomes. Avoiding excessive alcohol intake, maintaining a healthy body weight, exercising regularly, managing diabetes and cholesterol, getting vaccinated against hepatitis viruses, and avoiding unnecessary exposure to hepatotoxic chemicals all significantly reduce risk. For people already diagnosed with chronic liver disease, ongoing medical care, regular monitoring and adherence to treatment can slow or halt progression, enabling many individuals to live productive and meaningful lives despite their diagnosis.
Ultimately, chronic liver disease represents a gradual erosion of one of the body’s most essential organs, with consequences that reach far beyond the liver itself. It reflects a breakdown in metabolic stability, detoxification capacity, circulatory dynamics and immune balance. But it also reflects the resilience of the liver—one of the few organs capable of regenerating when given the right environment. The future of chronic liver disease management lies in early detection, targeted medical therapies, improved public awareness, and continued research into regenerative medicine and organ-preserving interventions. In this sense, chronic liver disease is both a challenge and an opportunity: a challenge because it threatens global health across diverse populations, and an opportunity because the liver’s regenerative potential gives clinicians and patients a chance to intervene before irreversible damage occurs.