Pancreas Anatomy – Structure, Location, Exocrine and Endocrine Functions, Digestive Support, Hormonal Regulation, Cellular Architecture, and Its Central Role in Human Metabolism and Health
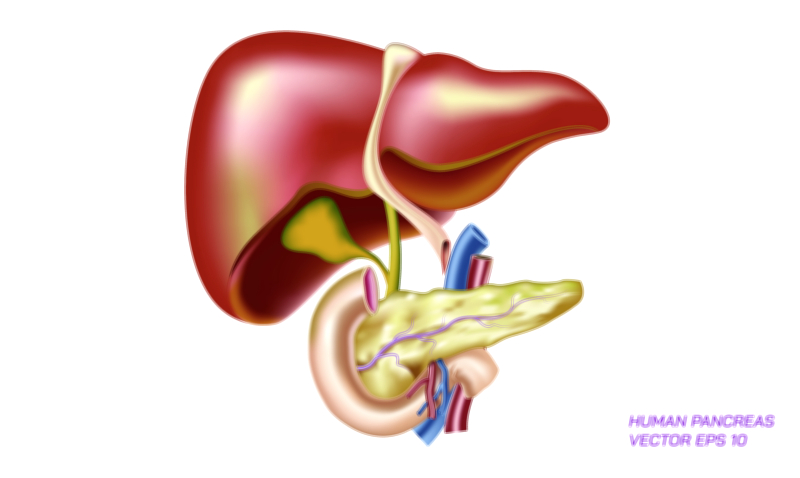
The pancreas is one of the most multifunctional and indispensable organs in the human body, serving as both a digestive powerhouse and a hormonal regulator that maintains metabolic balance with remarkable precision. Anatomically, it is a soft, elongated gland situated deep within the abdominal cavity, tucked behind the stomach and in front of the spine, extending horizontally from the curve of the duodenum on the right toward the spleen on the left. Its strategic location allows it to interact intimately with multiple organ systems, especially the liver, gallbladder, small intestine, and bloodstream. Nevertheless, the pancreas often remains unnoticed until disease disrupts its elaborate functions. Understanding its anatomy provides not only structural insight but also an appreciation for how seamlessly the body integrates digestion, nutrient absorption, and blood sugar regulation through a single organ that works quietly and continuously throughout life.
Anatomical Regions of the Pancreas and Their Structural Significance
The pancreas is divided into four main regions: the head, neck, body, and tail. The head of the pancreas nestles into the C-shaped curve of the duodenum, which is the first segment of the small intestine. This positioning is not accidental—it ensures that pancreatic secretions enter the digestive tract precisely where food first arrives from the stomach. The uncinate process, a projection from the head, curves behind major blood vessels, anchoring the gland securely. Moving leftward, the pancreas narrows into the neck, then expands into the elongated body that lies behind the stomach. Finally, the tail of the pancreas tapers toward the spleen. Running through the length of the gland is the main pancreatic duct, a delicate internal channel that merges with the bile duct before emptying into the duodenum. This structural arrangement ensures that pancreatic enzymes and bile—two critical digestive substances—reach the intestine in coordinated fashion. Even these directional details reveal the precision with which the digestive system is constructed.
Exocrine Pancreas and the Digestive Architecture of Acinar Cells and Ducts
Most of the pancreas is devoted to its exocrine function, meaning it produces and secretes substances externally into the digestive tract rather than directly into the blood. The exocrine component is made up of clusters of cells called acini, which synthesize and release a highly specialized digestive fluid containing enzymes that break down proteins, carbohydrates, and fats. These enzymes include amylase for starch digestion, lipase for fat digestion, and proteolytic enzymes such as trypsin and chymotrypsin for breaking down proteins. Each of these substances is produced in inactive form to prevent premature digestion of the pancreas itself, an evolutionarily crucial safeguard. The fluid produced by acinar cells travels through an intricate network of ducts, starting from tiny intercalated ducts that merge into larger ones until finally joining the main pancreatic duct. From there, pancreatic secretions are delivered into the duodenum precisely when food arrives, helping transform complex macromolecules into absorbable nutrients. This digestive contribution allows the body to extract energy, vitamins, and building blocks for cells from what would otherwise be biologically inaccessible food matter.
Endocrine Pancreas and the Hormonal Network of the Islets of Langerhans
While the exocrine system handles digestion, a smaller but equally vital portion of the pancreas carries out endocrine functions—hormonal regulation of metabolism. Scattered like islands among the acinar tissue are clusters of endocrine cells known as the islets of Langerhans. These microscopic structures contain several hormone-secreting cell types, each performing a distinct role in blood glucose regulation. Beta cells produce insulin, which lowers blood glucose by facilitating the uptake of glucose into cells for energy or storage. Alpha cells produce glucagon, which raises blood glucose by signaling the liver to release stored energy when blood sugar drops too low. Delta cells secrete somatostatin, a regulatory hormone that balances insulin and glucagon release and modulates digestive activity. PP (pancreatic polypeptide) cells influence appetite and digestive enzyme secretion. Each hormone circulates through the bloodstream rather than entering the digestive tract, demonstrating how closely the pancreas links digestion and energy metabolism. When this endocrine balance falters, serious health consequences arise; diabetes mellitus develops when insulin production or insulin responsiveness becomes impaired, underscoring how a tiny portion of pancreatic tissue has enormous power over overall metabolic health.
Integration of the Pancreas with Digestive and Metabolic Systems
The pancreas does not operate in isolation; rather, it exists as an integrated hub connecting digestive and endocrine networks. When a person eats, neural and hormonal signals inform the pancreas that food is entering the intestine. In response, exocrine cells release digestive enzymes, while endocrine cells monitor blood glucose changes. A meal rich in carbohydrates prompts a rapid insulin response, preventing dangerous spikes in blood sugar, while fasting stimulates glucagon secretion to maintain energy supply. The liver, intestine, gallbladder, and pancreas form a tightly interconnected metabolic circuit. Bile released from the gallbladder emulsifies fats, allowing pancreatic lipase to work efficiently. Carbohydrate digestion by pancreatic enzymes makes glucose available for immediate cellular use under the guidance of insulin. This sophisticated synergy reveals the pancreas as a conductor of metabolic orchestration rather than a simple gland.
Clinical Relevance and Vulnerability of the Pancreas
Despite its importance, the pancreas is vulnerable to several disorders that demonstrate how delicate its structural and functional equilibrium is. Pancreatitis occurs when digestive enzymes become activated prematurely within the pancreas, causing inflammation and self-digestion of tissues. This condition ranges from mild to life-threatening and often results from gallstones blocking the pancreatic duct or chronic alcohol use. Pancreatic cancer, though less common than cancers of the stomach or colon, remains one of the most dangerous due to its subtle early symptoms and deep anatomical placement, which delay detection. Diabetes—both type 1 and type 2—arises from endocrine dysfunction involving insulin deficiency or resistance. These disorders highlight that the pancreas is not only essential but also biologically fragile, requiring both protective anatomy and precise biochemical control to function safely.
Educational Significance of Studying Pancreas Anatomy
Learning and understanding pancreas anatomy illustrates some of the most important lessons in human biology. It teaches that digestion and metabolism are not separate processes but deeply interdependent mechanisms coordinated through one organ. It demonstrates how microscopic cell clusters can determine whole-body energy regulation. It shows that the layout of organs in the body is not random but engineered for functional efficiency. It also reveals how small disturbances—whether genetic, lifestyle-related, infectious, or inflammatory—can affect the entire body by interfering with pancreatic activity. Through studying the pancreas, students come to understand that maintaining health requires protecting the structure and function of organs that work silently in the background, ensuring that every cell receives both nutrients and energy to sustain life.
In the grand perspective of human physiology, the pancreas stands as a reminder that survival depends not only on what we eat but on how expertly the body converts food into biological fuel and regulates that fuel with precision. It is both a chemical factory and a hormonal decision-maker, able to operate continuously and adapt in real time to the body’s needs. The deeper one explores pancreatic anatomy, the more appreciation develops for the astonishing complexity of human biology and the quiet, constant labor performed by an organ that rarely receives attention until illness interrupts its essential work.