Normal Breathing, Asthma Episode, and Emergency Showing Airflow Restriction and Bronchial Changes in Human Lungs
Breathing is one of the most fundamental automatic functions of the human body, and under normal conditions, air flows in and out of the lungs with very little effort. The bronchial passages—the network of airways that branch throughout the lungs—remain open, flexible, and unobstructed, allowing oxygen to enter and carbon dioxide to be expelled smoothly. During quiet breathing, the airway walls are relaxed, the surrounding muscles are not constricted, and the inner lining of the bronchi produces only a thin layer of mucus necessary to keep the airways moist. When a diagram contrasts normal breathing with asthma episodes and asthma emergencies, the differences become stark: what is effortless in healthy lungs becomes increasingly difficult and even dangerous when inflammation, muscle tightening, and mucus buildup interfere with airflow. This progression from normal function to restricted airflow reveals why asthma is not simply a respiratory discomfort but a condition that requires careful understanding and quick intervention when symptoms escalate.
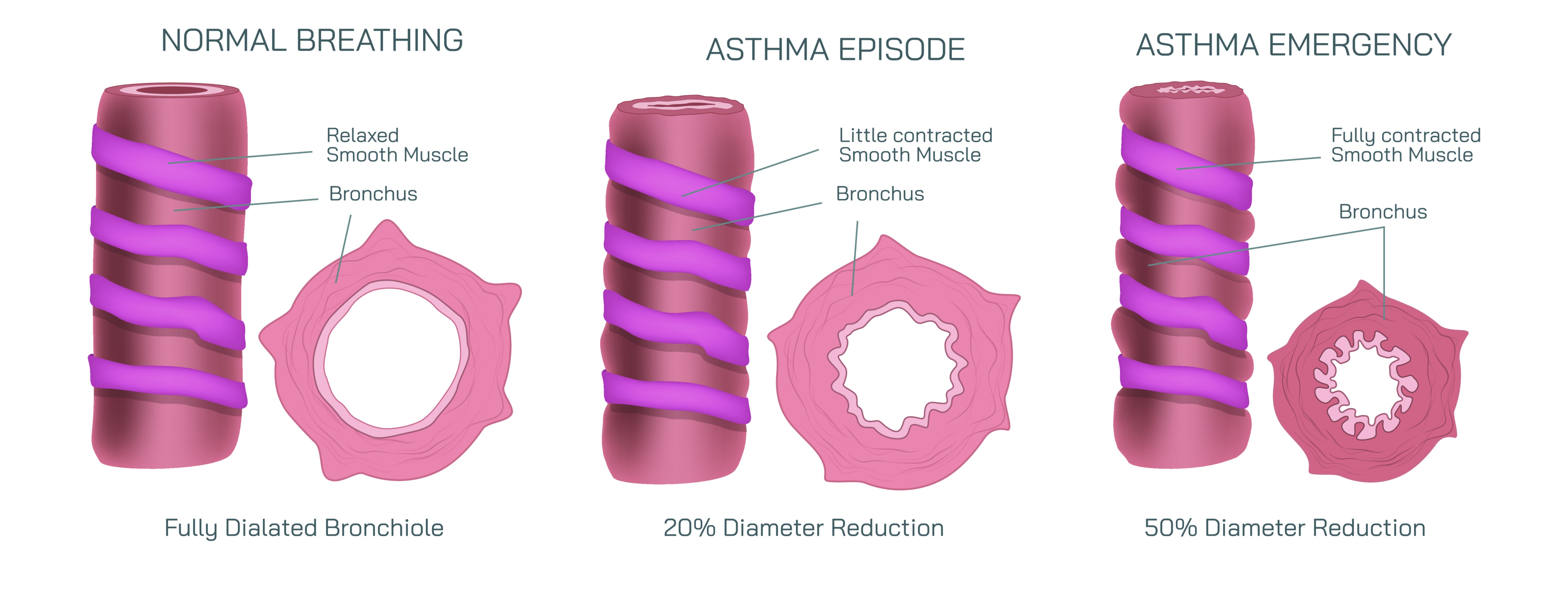
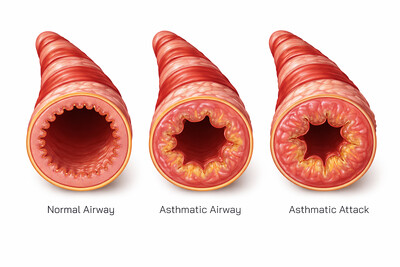
In normal breathing, the bronchial tubes are wide and unobstructed. Their walls maintain a balance of smooth muscle tone and flexibility, ensuring that each breath passes freely down to the alveoli—the tiny air sacs where oxygen exchange occurs. The lining of the bronchi remains thin and uninflamed, leaving plenty of space for air to travel. In a visual illustration, the open airway appears circular and symmetrical, with a large clear lumen and no excessive mucus. The passage is wide enough that even a strong inhalation or exhalation poses no resistance. This state represents the baseline for lung health, where the body receives oxygen efficiently and breathing remains quiet and effortless.
During an asthma episode, the environment inside the airways changes dramatically. Asthma is a chronic inflammatory respiratory disorder in which the bronchi become hypersensitive to triggers, including allergens, cold air, respiratory infections, exercise, stress, pollutants, and irritants such as smoke or dust. When exposed to triggers, the airway walls become inflamed and swollen, narrowing the passage through which air must travel. The smooth muscles surrounding the bronchi tense and begin to contract, a process known as bronchospasm, which further reduces the airway diameter. In addition to swelling and muscle tightening, the lining of the bronchi produces excess mucus that collects inside the narrowed space, adding yet another layer of obstruction. In an illustration, the airway during an asthma episode looks visibly restricted: the lumen (air passage) is smaller, the walls are thick and inflamed, and sticky mucus is present in significant amounts. Although air can still move through, it does so with difficulty, creating audible wheezing and causing the individual to feel short of breath, tight-chested, and fatigued.
Symptoms during an asthma episode vary in intensity but typically include coughing, wheezing, difficulty breathing, and chest tightness. Exhalation becomes especially difficult because air can enter the lungs more easily than it can exit through the narrowed passages. Some air becomes trapped inside, making subsequent breaths less effective and producing a sensation of not being able to fully empty the lungs. Even though the episode causes discomfort and distress, many individuals can manage this stage with inhaled bronchodilators—medications that relax the airway muscles and reopen the bronchial passages. Anti-inflammatory medications also help calm the swelling of the airway lining, reducing the frequency and severity of episodes.
An asthma emergency represents a dangerous escalation in this process and requires prompt medical attention. During an emergency, inflammation intensifies, the smooth muscles tighten dramatically, and mucus production increases to the point that airflow becomes critically low. At this stage, the airway lumen becomes extremely narrow—sometimes barely open—and the lungs struggle to deliver enough oxygen or release enough carbon dioxide. In a visual representation, the airway during an asthma emergency appears almost fully collapsed by swelling and muscle contraction, with thick mucus nearly filling the small remaining passage. Breathing becomes rapid, shallow, and labored, and the individual may use accessory muscles in the neck and chest to try to pull in air. Speaking may become difficult or impossible, and anxiety increases as the body reacts to oxygen deprivation. In severe cases, wheezing may disappear—not because airflow has improved, but because so little air is moving through the airways that the sound of wheezing is no longer produced. This silent chest stage is a critical medical warning sign.
The consequences of this restricted airflow affect not only the lungs but the entire body. Without adequate oxygen, the brain, heart, and other vital organs struggle to function. Carbon dioxide builds up in the bloodstream, altering pH levels and risking respiratory failure. A person experiencing an asthma emergency requires urgent medical treatment, often including high-dose bronchodilators, corticosteroids, oxygen support, and in severe cases, ventilatory assistance. The goal is rapid reversal of airway narrowing before the situation progresses to life-threatening oxygen deprivation.
The physiological changes that drive asthma symptoms are deeply rooted in immune activity. Asthma is characterized by an overactive inflammatory response in the airways, where immune cells release chemical mediators that trigger swelling and mucus secretion. Over time, repeated airway inflammation can contribute to airway remodeling, a long-term structural change that may make airways thicker and less flexible, meaning airway hyperreactivity may worsen if asthma is not well controlled. This highlights why asthma management focuses not only on treating acute symptoms but also on preventing chronic inflammation through long-term medical therapy, trigger avoidance, and regular monitoring.
Understanding the transition from normal breathing → asthma episode → asthma emergency is essential for recognizing the early warnings of worsening symptoms and intervening before airflow becomes critically restricted. Normal breathing represents open, relaxed airways with effortless airflow. An asthma episode represents narrowed, inflamed airways with restricted airflow that still responds to quick-relief medications. An asthma emergency represents a dangerously constricted airway system in which airflow becomes so limited that oxygen supply to the body is threatened.
In a medical diagram, these three states create a powerful story:
Normal airway: wide open lumen, relaxed smooth muscles, minimal mucus
Asthma episode airway: swollen lining, tight muscles, increased mucus narrowing the passage
Asthma emergency airway: severely contracted airway, thick mucus, dangerously obstructed airflow
The lungs are not simply mechanical sacks of air—they are living immune-regulated organs whose function depends on the fluid balance between inflammation, muscle tone, mucus production, and environmental exposure. When asthma disrupts this balance, the effects are immediate and dramatic. A clear visual depiction of these stages helps patients, medical learners, and caregivers understand what is happening inside the lungs during an asthma attack and why rapid treatment and long-term management are essential for maintaining safe and healthy breathing.