Stress Response System — Human Body Reaction to Physical and Emotional Stressors Explained
The stress response system is one of the most remarkable defense mechanisms in the human body, designed to protect us from danger, maintain internal stability, and help us adapt to changing environments. When the brain perceives a threat—whether physical, emotional, psychological, or even imagined—it instantly activates a coordinated biological reaction known as the stress response. This reaction prepares the body to cope with the perceived challenge by sharpening awareness, boosting energy availability, altering bodily priorities, and mobilizing physiological resources. This process is not random; it involves precise interactions between the nervous system, the endocrine system, and the immune system, all working together in a highly synchronized survival mechanism. At the heart of this process lie two major pathways: the rapid fight-or-flight response triggered by the sympathetic nervous system and the longer-duration hormonal response coordinated through the hypothalamus–pituitary–adrenal (HPA) axis. Together, these pathways determine how humans experience and respond to stress in daily life, whether encountering immediate threats such as danger or prolonged stressors such as financial worries, interpersonal conflicts, work pressure, emotional trauma, or chronic uncertainty.
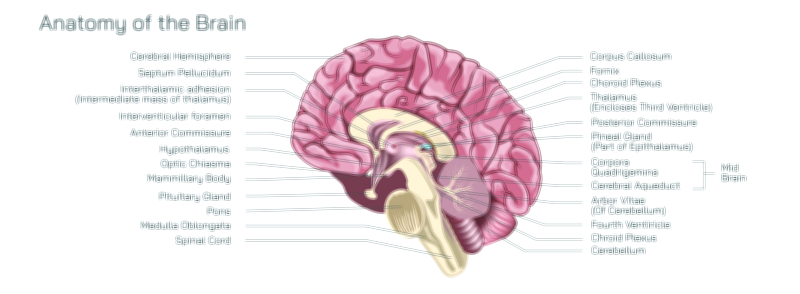
The activation of the stress response begins in the brain’s emotional processing center, the amygdala. When the amygdala interprets a situation as threatening, it sends an emergency signal to the hypothalamus, which acts as the command center for stress management. The hypothalamus rapidly activates the sympathetic nervous system, triggering the adrenal medulla to release adrenaline and noradrenaline into the bloodstream. These hormones cause a surge of physiological changes that collectively form the fight-or-flight state. Heart rate increases rapidly to pump more blood to skeletal muscles, breathing accelerates to supply additional oxygen, and blood vessels in the digestive and reproductive organs constrict so that energy can be redirected to systems required for survival. Pupils dilate to sharpen vision, reflexes become quicker, and heightened alertness narrows focus toward the threat. Blood glucose and fatty acids are released into circulation to provide instant energy. In this moment, the body prioritizes survival above all else and temporarily halts processes that are not immediately essential, including digestion, growth, tissue repair, and reproductive functions. These changes unfold within seconds, reflecting the evolutionary purpose of the stress response—to provide the physical and mental readiness required to escape danger, defend oneself, or endure a sudden challenge.
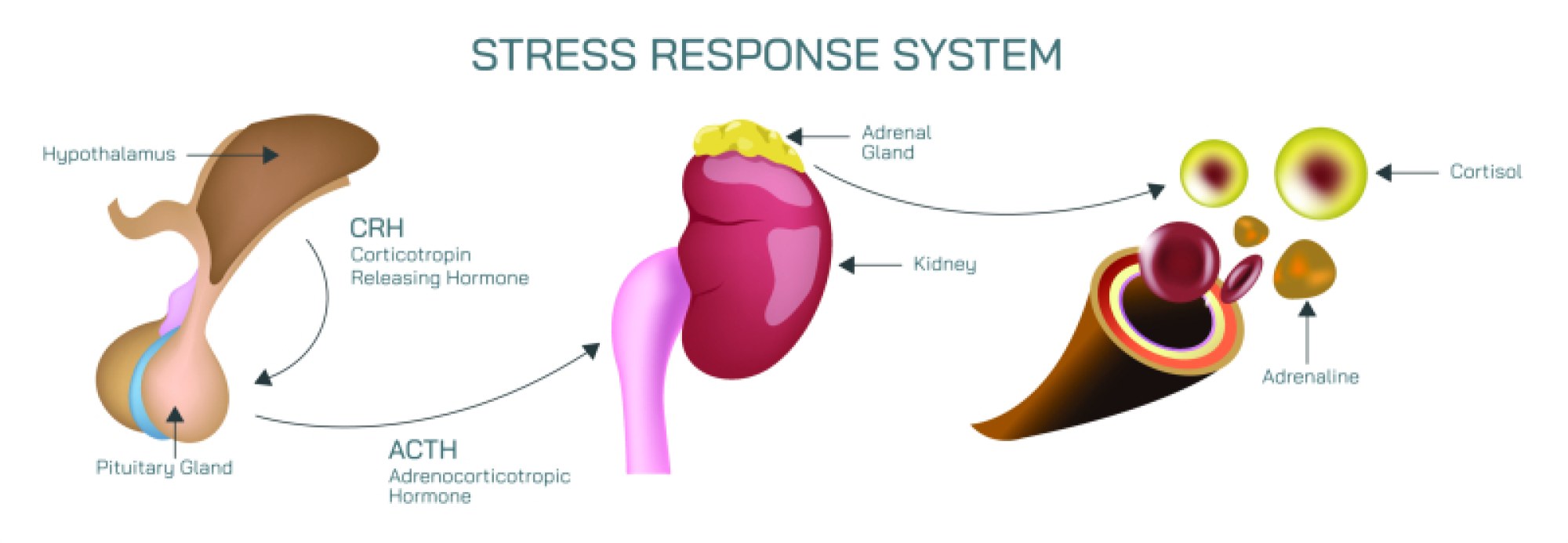
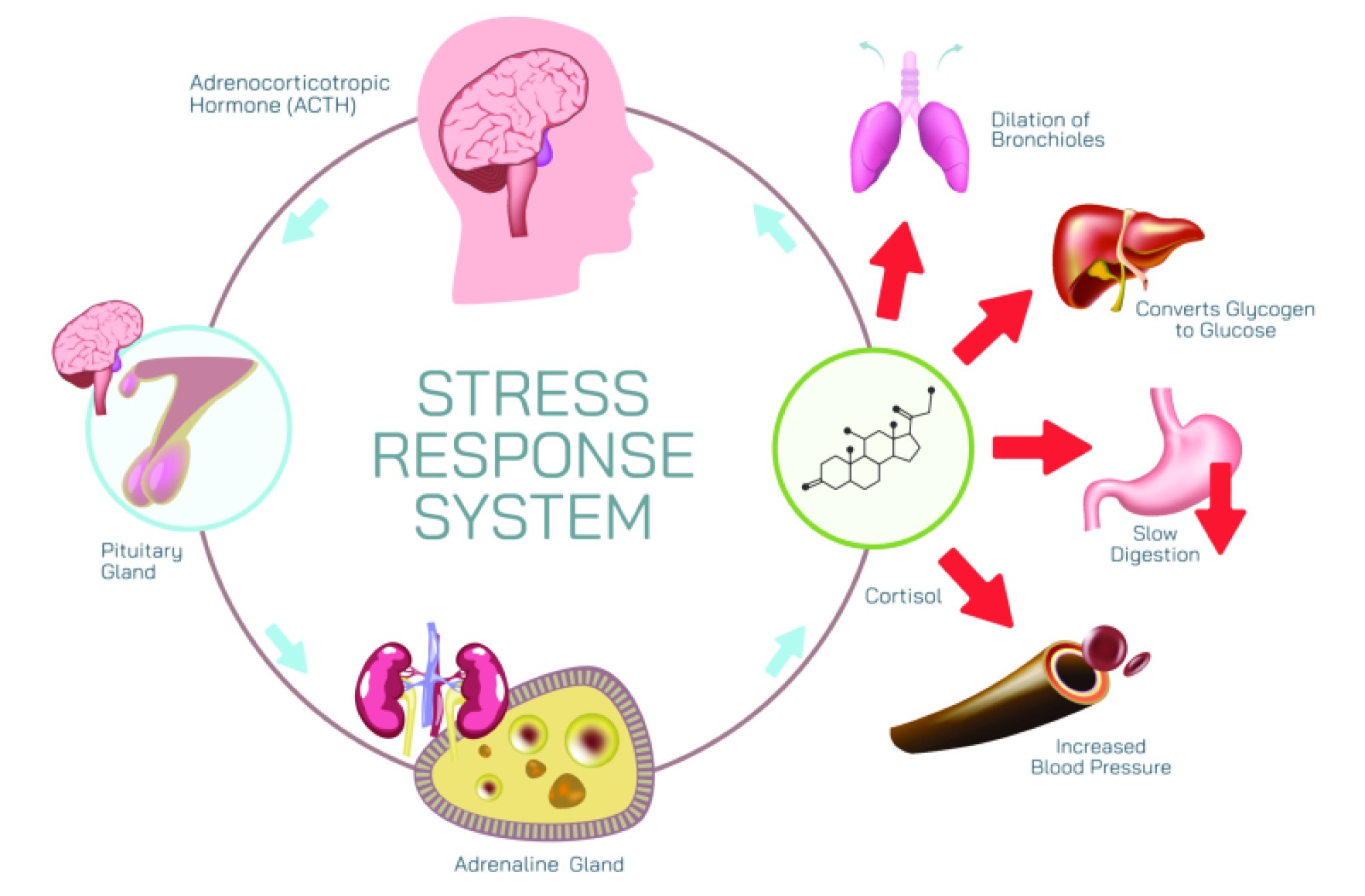
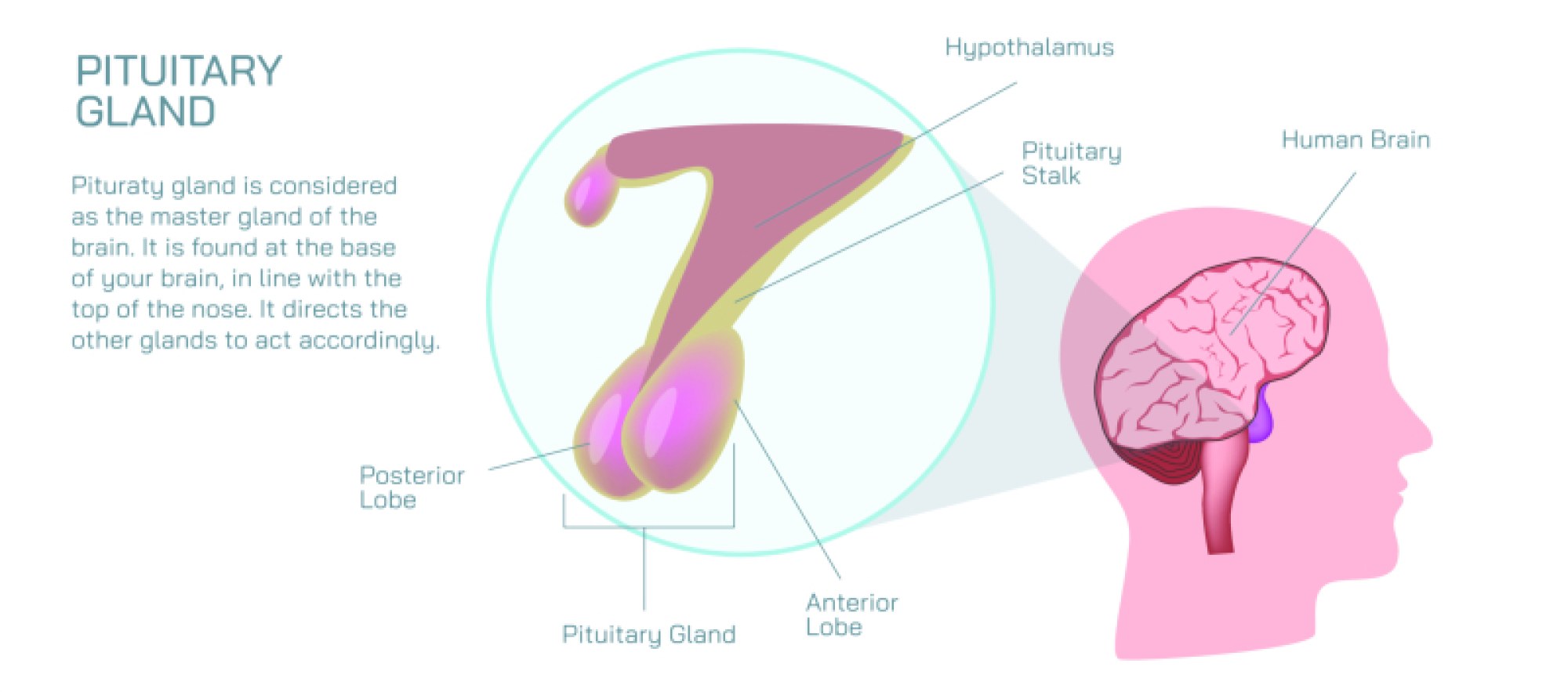
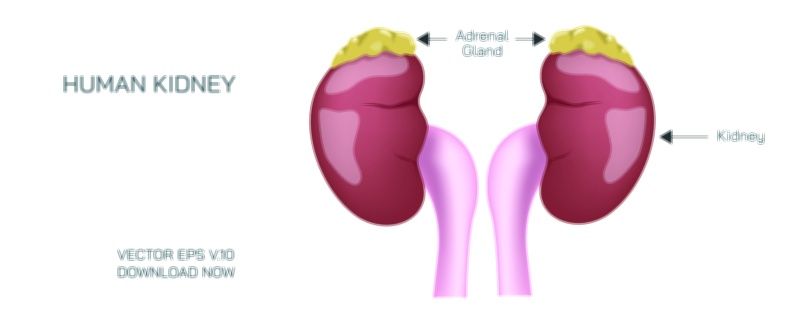
If the stressor persists beyond the initial surge, the body transitions into the HPA axis response, a longer-term stress management system that keeps the body prepared for sustained pressure. The hypothalamus releases corticotropin-releasing hormone (CRH), signaling the pituitary gland to secrete adrenocorticotropic hormone (ACTH), which then triggers the adrenal cortex to release cortisol, the primary stress hormone. Cortisol maintains high blood sugar for energy, increases blood pressure to assist perfusion, and suppresses inflammation temporarily to prevent excess immune activity during crisis. This hormone fundamentally changes how the body operates, shifting metabolism away from long-term maintenance and toward short-term survival. In moderate levels and for limited periods, cortisol is beneficial—supporting endurance, stabilizing alertness, improving memory for relevant details, and enabling the body to withstand demanding conditions. However, the body intends for cortisol levels to decline once the stressor ends. When stress becomes prolonged or repeated without recovery, cortisol remains chronically elevated and begins to produce harmful effects, transforming a useful adaptive response into a biological burden.
While acute stress protects life, chronic stress slowly deteriorates health because the body cannot remain in survival mode indefinitely without consequences. Long-term cortisol overexposure disrupts sleep cycles, destabilizes appetite, increases abdominal fat storage, weakens immune defenses, and impairs cardiovascular and metabolic functioning. The digestive system experiences reduced blood flow and enzyme activity, leading to issues such as acidity, irritable bowel syndrome, and nutrient absorption difficulties. Reproductive hormone production declines, sometimes affecting fertility, libido, and menstrual regularity. Chronic activation of the nervous system leads to persistent muscle tension, headaches, back pain, and increased sensitivity to pain signals. Cognitively, prolonged stress impairs memory, concentration, and decision-making, as the prefrontal cortex—the brain region responsible for logic and planning—begins to lose regulation over the amygdala. Emotionally, stress can lead to irritability, anxiety, impulsivity, low motivation, sadness, and feelings of overwhelm. The immune system, once empowered by short bursts of stress, becomes suppressed with chronic exposure, leaving the body more vulnerable to infections, slower wound healing, and increased inflammation. Over time, chronically elevated stress levels become a contributing factor to numerous physical and mental health conditions including hypertension, depression, diabetes, autoimmune disorders, and cardiovascular disease.
A critical but often overlooked aspect of the stress response system is that the human brain reacts not only to true physical threats but also to psychological stressors and imagined scenarios. Worries about the future, self-criticism, social pressure, work deadlines, financial strain, unresolved trauma, and uncertainty activate the same pathways as physical danger. The brain does not differentiate between an approaching predator and anxiety about an exam, as both are interpreted as threats requiring a defensive response. This explains why the modern world, filled not with physical dangers but with cognitive and emotional pressures, can overstimulate the stress response and overload the HPA axis. At the same time, different individuals have very different sensitivity levels to stress because the brain’s appraisal system—how it interprets experiences—is shaped by genetics, childhood environments, social support, self-esteem, coping skills, belief systems, and past trauma. Two people can experience the same external situation but have completely different stress reactions because the determining factor is perception rather than the event itself.
Despite the negative effects of chronic stress, the stress response system is not inherently harmful. It becomes damaging only when activated excessively or without relief. Stress is a survival mechanism designed not just for crisis but for learning and adaptation. Short bursts of stress can enhance performance during challenges such as exams, competitions, public speaking, or problem-solving. In moderation, stress boosts motivation, sharpens focus, and strengthens resilience. The key to long-term well-being lies in the body’s ability to move fluidly between activation and recovery. Recovery states—such as deep sleep, relaxation, social bonding, physical activity, creative expression, meaningful connection, and periods of safety—allow the parasympathetic nervous system to counterbalance stress. This “rest-and-digest” system lowers heart rate, restores digestion, regulates immune function, promotes tissue repair, and reduces cortisol levels. A healthy nervous system oscillates between stress and recovery rather than remaining locked in one mode.
Ultimately, mastering stress does not mean eliminating it from life, but regaining control over the stress response rather than allowing it to dominate behavior and health. The nervous system learns through experience, and over time the brain can form healthier automatic responses to pressure. Habits such as regular physical exercise, deep breathing, mindfulness, adequate sleep, social connection, emotional expression rather than suppression, realistic goal-setting, and maintaining boundaries help the body shift from chronic activation into balance. Strengthening the prefrontal cortex through self-awareness and deliberate decision-making reduces amygdala reactivity and improves emotional regulation. Even simple awareness—recognizing when the stress response has been triggered—weakens its control because it brings the decision-making brain back online. The goal is not to live without stress but to develop the resilience to move in and out of stress with control rather than struggle, using the stress response not as a force that damages health but as one that supports adaptation, strength, safety, and meaningful performance. When the stress response system is understood and managed wisely, it becomes not a source of suffering but a biological ally that helps humans navigate challenges, recover from adversity, and thrive in demanding environments.