Thyroid Gland Anatomy – Structure, Location, Microscopic Architecture, Hormone-Secreting Cells, Vascular and Neural Connections, and Its Role as a Central Organ of the Endocrine System
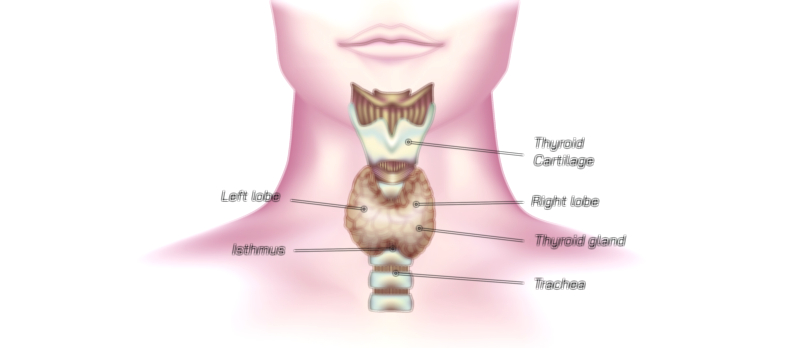
The thyroid gland is a small but critically important endocrine organ responsible for regulating metabolism, growth, and energy utilization throughout the human body. Situated in the anterior region of the neck, it lies just below the larynx and wraps around the upper trachea like a shield, which is reflected in its name—derived from the Greek word thyreos, meaning “shield.” Externally, the thyroid appears as a butterfly-shaped structure composed of two distinct lobes, the right and left, which are connected at the midline by a narrow tissue bridge called the isthmus. In many individuals, a small pyramidal lobe extends upward from the isthmus, a remnant of embryological development showing the migration of thyroid tissue from the tongue base to its final location in the neck. The gland is soft, smooth, and highly vascularized, reflecting its role in rapidly releasing hormones into the bloodstream.
Macroscopic Structure and Relationship With Nearby Neck Anatomy
The thyroid rests in the visceral compartment of the neck, deep to the infrahyoid (“strap”) muscles and superficial to the trachea. Each lobe extends superiorly toward the thyroid cartilage and inferiorly toward the suprasternal notch. During swallowing, the thyroid moves upward because of its attachment to the larynx via connective tissue, a feature that assists in clinical examination. Posterior to the thyroid lie the parathyroid glands—typically four, though their number may vary—which control calcium metabolism independently of the thyroid. The recurrent laryngeal nerves, responsible for controlling vocal cord movement, run very close behind the thyroid lobes, which is clinically significant because thyroid enlargement or surgical procedures can affect speech if these nerves are irritated or injured. The thyroid’s arterial supply is rich and includes the superior thyroid arteries (branches of the external carotid) and inferior thyroid arteries (branches of the thyrocervical trunk), with possible contribution from the thyroid ima artery in some individuals. Venous drainage occurs through superior, middle, and inferior thyroid veins, reflecting the gland’s need for rapid hormonal transport.
Microscopic Anatomy and Functional Unit: The Thyroid Follicle
The thyroid gland’s function is governed by its microscopic structure. The gland is composed of thousands of spherical units called follicles, each of which acts as a self-contained center for hormone storage and release. A follicle consists of a central cavity filled with colloid, a viscous material primarily composed of thyroglobulin, which stores the building blocks of thyroid hormones. Surrounding each colloid sphere is a layer of epithelial cells known as follicular cells or thyrocytes. These specialized cells absorb iodine from the bloodstream, attach it to tyrosine residues within thyroglobulin, and later break down the colloid matrix to release the active hormones thyroxine (T4) and triiodothyronine (T3) into circulation when stimulated. T3 is the biologically more active form, while T4 serves as the major circulating precursor that tissues convert to T3 as needed.
Another important cell population within the thyroid is the parafollicular or C cells, found in the spaces between follicles. These cells secrete calcitonin, a hormone that plays a role in regulating calcium levels by promoting calcium deposition in bone and lowering serum calcium concentrations when levels become high. Although calcitonin is not the primary regulator of calcium in adults, the presence of C cells shows that the thyroid contributes not only to metabolic regulation but also to mineral homeostasis.
Endocrine Regulation and Feedback Mechanism
4. Once these hormones reach optimal levels in the bloodstream, they provide negative feedback to both the pituitary and hypothalamus, reducing TSH and TRH secretion and preventing excessive thyroid stimulation. This system enables the thyroid to adjust metabolic output in response to environmental conditions such as cold exposure, growth, stress, pregnancy, and nutritional changes.
Functions of Thyroid Hormones in Whole-Body Physiology
The hormones produced by the thyroid have wide-reaching effects throughout the body. They increase the basal metabolic rate by stimulating cellular energy production, regulate body heat by controlling oxidative mechanisms, influence heart rate and cardiac output, accelerate digestion and gastrointestinal motility, and support protein synthesis and tissue growth. In developing fetuses and young children, thyroid hormones are vital for brain development, skeletal maturation, and cognitive function. Because nearly every cell contains receptors for T3, thyroid function is essential for maintaining physical and mental vitality. When thyroid hormone production is disrupted—either too high or too low—the effects cascade into multiple organs and systems, explaining why thyroid disease manifests with such diverse symptoms.
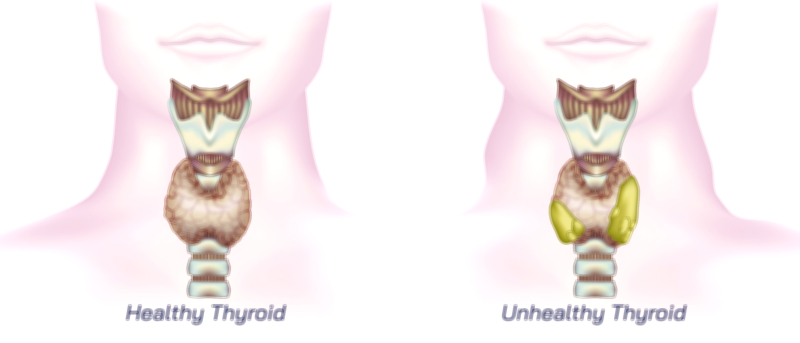
Clinical Relevance: What Happens When Thyroid Anatomy Is Altered
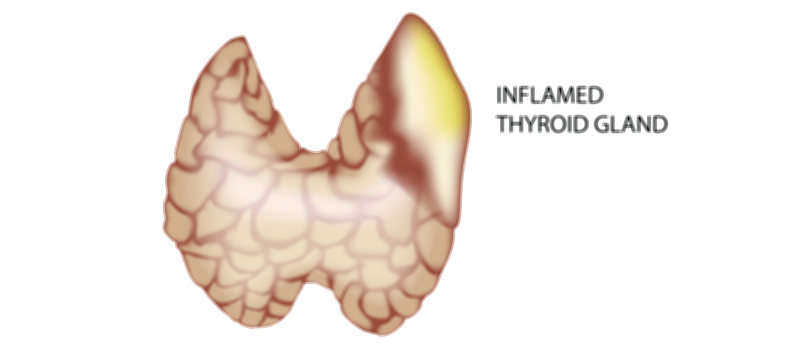
Even minor anatomical disturbances in the thyroid can have large physiological consequences. Enlargement of the thyroid (goiter) may arise from iodine deficiency, autoimmune inflammation, hormonal dysregulation, or nodular overgrowth. Nodules may form within the gland, either benign or malignant, and can interfere with uniform hormone production. Autoimmune destruction of thyroid tissue can lead to hypothyroidism, whereas autoimmune overstimulation can lead to hyperthyroidism. Thyroid cancer alters both the microscopic and macroscopic architecture of the gland, disrupting hormone function and often requiring surgical removal, radioactive iodine, or lifelong hormone replacement. Because of its close anatomical relationship with the trachea, esophagus, parathyroid glands, and recurrent laryngeal nerves, changes in thyroid structure can affect swallowing, breathing, calcium balance, and voice quality.
Educational Importance and the Thyroid’s Place in Human Anatomy
The anatomy of the thyroid illustrates the powerful relationship between structure and function in the endocrine system. It demonstrates how a compact organ composed of repeating microscopic units can control metabolism for the entire body, and how hormone regulation depends on feedback loops rather than moment-to-moment neural input. Studying the thyroid highlights the vulnerability of endocrine organs to immune attack, the importance of dietary iodine, and the delicate balance necessary for optimal metabolic performance. It also teaches that physical examination of the neck, laboratory testing of hormone levels, and imaging of gland structure must be understood together to evaluate thyroid health accurately.
Ultimately, the thyroid gland represents a convergence of anatomy, physiology, biochemistry, and systemic health. Its precise placement in the neck enables efficient hormonal supply to the bloodstream, its microscopic follicles provide a sophisticated storage and release mechanism, and its hormones sustain life by regulating energy at the cellular level. Through its anatomy, students and clinicians gain a deeper appreciation for how even small structures in the human body play essential roles in the continuity of health and metabolic stability.