Stomach Ulcer and Disease – Understanding Ulcer Formation, Gastric Lining Damage, Digestive Symptoms, Causes, Complications, Diagnosis, Treatment, and Educational Insight for Prevention and Long-Term Stomach Health
Stomach ulcers, medically known as gastric ulcers, represent one of the most widely recognized yet frequently misunderstood stomach diseases. A stomach ulcer is not simply an irritation or common acidity problem; it is an open sore that develops when the protective lining of the stomach becomes damaged and unable to defend itself against naturally occurring gastric acid. The stomach constantly produces acid to digest food, but under normal circumstances, a thick layer of mucus protects the stomach lining from injury. When this balance breaks down—because of infection, medication, lifestyle factors, or biological vulnerability—the acid begins to erode the tissue beneath. Over time, this erosion deepens into an ulcer. Understanding stomach ulcers from a medical education standpoint involves not only learning what they are but also how they form, why they cause symptoms, how they are diagnosed, and most importantly, how they can be treated and prevented. Stomach disease connected to ulcers offers a clear lesson about the delicate equilibrium inside the digestive system: too much acid is harmful, too little protection is harmful, and healing depends on restoring this equilibrium rather than merely suppressing symptoms.
A major breakthrough in ulcer research came with the recognition that infection by Helicobacter pylori (H. pylori) is the leading cause of stomach ulcers worldwide. For decades, ulcers were believed to stem mainly from stress and diet until scientists discovered that this spiral-shaped bacterium can survive in the stomach’s acidic environment by burrowing into the protective mucus layer. Once established, H. pylori triggers inflammation in the lining, weakens the mucus barrier, and makes the tissue more vulnerable to acid damage. Not everyone infected with H. pylori will develop ulcers, but the infection remains one of the most important risk factors. Education about this bacterium is crucial because many people experience chronic stomach discomfort for years without realizing that it is the result of an infection that can be treated permanently. Detection and eradication of H. pylori can eliminate the cause of ulcer formation rather than merely relieving symptoms temporarily.
Another major cause of stomach ulcers is the prolonged use of non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, aspirin, and naproxen. These medications block the body’s production of prostaglandins, substances that protect the stomach from acid damage by strengthening the mucus barrier and improving blood flow to the lining. When prostaglandins are suppressed, the stomach becomes more vulnerable, and acid begins damaging the tissue. Individuals who take NSAIDs daily for chronic pain, arthritis, migraines, or injury—especially on an empty stomach—are significantly more likely to develop ulcers. The educational message here is that pain relievers are not harmless when misused. Many people assume they are safe because they do not require a prescription, yet long-term, unmonitored use may silently harm the stomach. Patients who require NSAIDs for medical reasons should be educated about taking them with food, avoiding excessive doses, and consulting healthcare providers about protective stomach medications if long-term use is necessary.
Alongside infection and medication effects, lifestyle habits also play a role in stomach disease and ulcers. While stress and diet alone rarely cause ulcers on their own, they intensify symptoms and delay healing. Smoking reduces blood supply to the stomach lining and slows tissue repair, making ulcers more likely to form and slower to heal. Excessive alcohol intake weakens the stomach lining, increases acid production, and worsens inflammation. Highly acidic or spicy foods do not directly cause ulcers, but they can aggravate existing ones and trigger pain in individuals with a vulnerable stomach lining. Emotional stress can worsen symptoms by altering digestive patterns, increasing sensitivity to pain, and interfering with appetite and sleep, all of which contribute to sickness cycles. Educational understanding helps individuals avoid blaming a single food or emotion for ulcers but instead appreciate how multiple influences combine to make the stomach more susceptible or more resistant to injury over time.
The symptoms of a stomach ulcer often overlap with symptoms of common digestive disturbances, creating confusion and delayed diagnosis. Most ulcers cause upper abdominal pain, usually between the ribs and the navel. The pain may be burning, dull, gnawing, or sharp, and it may fluctuate in cycles. Some individuals feel pain shortly after eating because food stimulates acid production, while others feel relief when they eat because food temporarily buffers the acid. Symptoms can also include bloating, nausea, loss of appetite, unexplained fullness, burping, heartburn, and unintentional weight loss. In some cases, pain may be absent even when an ulcer is present, especially in elderly individuals or those taking pain medication. This variety of symptom patterns highlights why medical evaluation is necessary when digestive discomfort persists. Many people attempt to treat ulcer pain with antacids or by limiting meals, but self-treatment may mask symptoms without resolving the underlying cause. Education teaches that persisting or recurrent stomach symptoms should not automatically be blamed on “acidity” or “gas” when they may represent tissue injury that requires targeted therapy.
A small number of ulcers progress to serious complications, which is why prompt recognition and treatment are essential. Bleeding ulcers can cause black, tar-colored stool, vomiting of blood, fatigue, and dizziness due to anemia. Perforated ulcers occur when the acid eats completely through the stomach wall, allowing stomach contents to spill into the abdominal cavity—a life-threatening emergency marked by sudden, intense abdominal pain. Obstructive ulcers can form near the exit of the stomach, blocking the passage of food and causing persistent vomiting, fullness, and inability to tolerate meals. These complications are uncommon but demonstrate that ulcers are not merely irritations; they are wounds that can worsen if left untreated. The more individuals understand the early warning signs, the more preventable these complications become.
Diagnosis of ulcers typically involves endoscopy, in which a small flexible camera is inserted through the mouth into the stomach to directly visualize the ulcer and evaluate its severity. Endoscopy is the most reliable method because it allows doctors to see the ulcer clearly, assess the surrounding tissue, and take samples to test for H. pylori. Other diagnostic tools include breath tests, stool tests, and blood tests to detect infection. In some cases, imaging studies such as X-rays or CT scans may be used when complications are suspected. From an educational standpoint, diagnosis provides relief and clarity because it replaces uncertainty with understanding and ensures that treatment addresses the true cause rather than only symptoms.
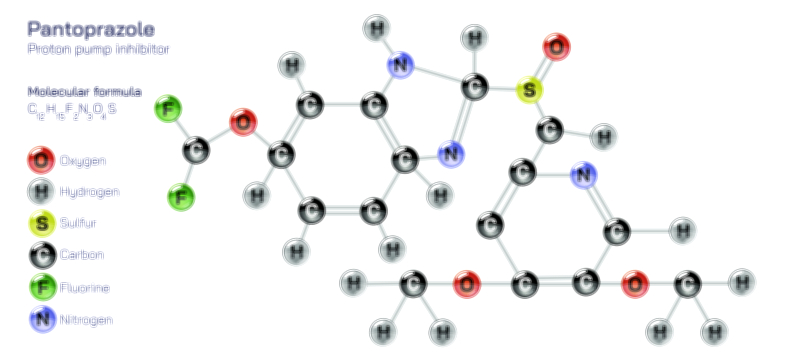
Treatment of stomach ulcers depends on the cause, and this principle is one of the most important lessons in digestive medicine. When H. pylori infection is responsible, antibiotic therapy combined with acid-reducing drugs is required to cure the ulcer. When NSAIDs are the cause, discontinuing or reducing the medication allows the stomach lining to heal, often with the help of proton pump inhibitors (PPIs) to reduce acid. Acid-suppressing medications alone can heal most ulcers within weeks, but only if the underlying cause is controlled. For smoking-related or alcohol-related ulcers, healing depends not only on medication but also on behavior modification that protects the stomach from recurring injury. Diet during ulcer treatment is not about rigid restrictions but about choosing foods that soothe rather than irritate: softer meals, reduced spices, low-acid beverages, high hydration, and regular eating patterns. Education empowers patients to understand that healing is cooperative—a partnership between medical treatment and self-care choices.
Prevention of ulcers offers meaningful insight into everyday digestive health. Anyone who learns about ulcers gains awareness of how powerful small habits can be. Eating slowly, avoiding overeating, spacing large meals, reducing alcohol and smoking, using NSAIDs cautiously, managing stress through healthy coping strategies, staying hydrated, and responding early to persistent digestive discomfort all help maintain a strong stomach lining. For individuals with H. pylori risk or history of ulcers, early screening during recurring stomach symptoms can prevent long-term disease. Prevention is not about fear but about recognizing how the stomach protects the rest of the body—and how daily choices protect the stomach in return.
Ultimately, understanding stomach ulcers as a disease transforms the way people interpret digestive discomfort. Rather than viewing stomach problems as random, mysterious, or insignificant, individuals learn to see the stomach as a sensitive but resilient organ that reacts to infection, medication, lifestyle, and emotional stress. Pain and discomfort are not punishments but signals calling for attention. The strongest message of medical education is that ulcers are highly treatable and often curable—especially when diagnosed early and treated correctly. Knowledge gives individuals confidence to seek care when needed, make informed choices about medication and diet, and support long-term stomach health through thoughtful, preventive habits.