Stomach Complication Medication – Understanding Treatment Approaches, Drug Categories, Mechanisms of Action, and Educational Insight for Safe Digestive Health Management
Stomach complications are among the most frequently treated medical concerns worldwide, and the medications used to manage them play a central role in both relief and prevention. Yet many people use stomach-related medicines without truly understanding what they treat, how they work, or when they should and should not be used. Some patients take acid-suppressing tablets for gas, antibiotics for viral infections, laxatives for mild bloating, or painkillers on an empty stomach without realizing these choices can worsen symptoms rather than solve them. Education about stomach complication medications is therefore essential not only to improve symptom relief but also to prevent misuse that may lead to dependency, rebound effects, resistant infections, or long-term digestive imbalance. The stomach depends on tightly coordinated chemical and muscular functions, and when disease, lifestyle habits, infection, or stress interfere, the resulting complications range from acidity and gastritis to constipation, diarrhea, ulcers, reflux, cramping, and chronic inflammation. Each problem demands a specific category of medication, and understanding why doctors choose certain medicines—and avoid others—is a powerful step toward safe digestive health.
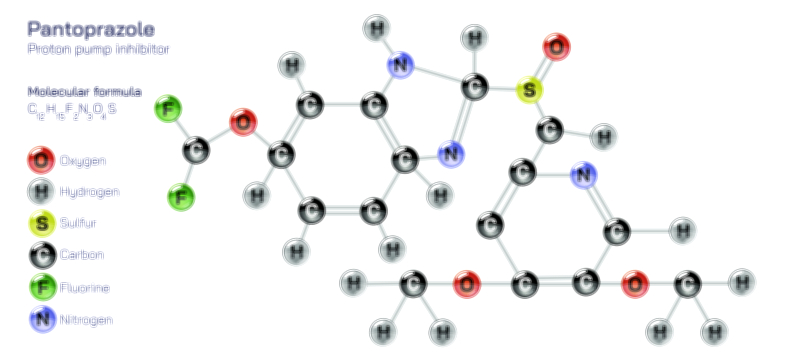
A foundational category of stomach complication medications involves acid regulation. The stomach naturally produces hydrochloric acid to break down food and kill harmful microbes, yet excess acid or misplaced acid can cause burning pain, reflux, sour taste, nausea, or gastritis. To manage this, medications fall into different subgroups based on how they act inside the body rather than simply suppressing discomfort. Antacids provide rapid but short-term relief by neutralizing existing acid. They work almost instantly because they act directly on the acid already present in the stomach, yet their effects fade quickly and do not treat deeper inflammation. H2 blockers reduce acid secretion by blocking the receptors that stimulate acid-producing cells, giving longer relief than antacids and often improving symptoms overnight. Proton pump inhibitors (PPIs) go one step further by switching off the final stage of acid production, making them the most powerful and longest-acting medicines for persistent reflux, gastritis, or ulcers. While these medications are extremely effective when appropriately used, the way they act explains why medical guidance is required. Overuse of antacids can disturb natural digestive acidity, long-term dependence on H2 blockers can reduce effectiveness over time, and excessive PPI use without medical supervision can interfere with nutrient absorption and normal acid protection. Education therefore encourages thoughtful use: acid-suppressing medications should solve the problem rather than become a habit.
Another major category of medications used for stomach complications is aimed at treating infections and inflammation. One of the most common causes of chronic gastritis and peptic ulcer disease is infection by the bacterium Helicobacter pylori, and this specific infection does not improve with antacids or PPIs alone. Instead, a carefully selected combination of antibiotics is required to eliminate the bacteria, often paired with PPIs to allow the stomach lining to heal. Patients who understand this link are more likely to follow the full treatment course and less likely to stop therapy as soon as symptoms improve, which is crucial for avoiding resistant infection. On the other hand, taking antibiotics without evidence of H. pylori or a bacterial cause of diarrhea can worsen stomach complications rather than improve them. Viral stomach infections, which are extremely common, do not benefit from antibiotics; instead, treatment involves hydration and rest. Recognizing the difference between infections requiring antibiotics and those that do not prevents medication misuse and protects long-term digestive well-being.
Another important class of stomach medications includes drugs that influence intestinal motility—how fast or slow the digestive system moves food forward. When intestinal movement becomes too rapid, diarrhea develops; when it becomes too slow, constipation follows. Medications are available to correct either imbalance, yet understanding how they work helps people use them safely. Anti-diarrheal medicines slow intestinal motility or reduce secretion into the bowel, allowing the body to reabsorb water and firm up stool. These drugs can be lifesaving in cases of chronic diarrhea or excessive fluid loss but must be used with caution. If diarrhea is caused by a bacterial toxin or food poisoning, slowing the bowel can trap the infection inside, making the illness worse. Conversely, constipation medications can relieve discomfort and heaviness by softening stool, increasing water content in the bowel, or stimulating intestinal movement. They are very effective, but long-term excessive use of stimulant laxatives can lead to dependency, weakening the bowel’s natural movement over time. For this reason, medical guidance often emphasizes hydration, physical activity, fiber intake, and gradual lifestyle adjustments alongside medication rather than immediate reliance on laxatives for every episode of constipation. Education helps patients understand that medications can support bowel rhythms, but the digestive system functions best when strengthened through healthy habits rather than constantly pushed by drugs.
Medications for gas, bloating, and indigestion form another important category in the treatment of stomach complications. These medicines do not reduce acid or alter bowel movement but rather help break up trapped gas bubbles, improve digestion of certain foods, or relax the digestive muscles. Simethicone-based medicines reduce surface tension on gas bubbles, making them easier to pass without pain. Digestive enzyme supplements help break down nutrients that some individuals cannot efficiently digest on their own, such as dairy sugar in lactose intolerance, fat in pancreatic insufficiency, or complex carbohydrates in some digestive sensitivities. Antispasmodic drugs reduce intestinal muscle spasms and pain during cramping episodes, particularly useful in individuals with irritable bowel sensitivity. Each of these medications works best when used for the correct digestive cause, showing why diagnosis matters. Someone who takes antacids for gas or laxatives for indigestion may not only fail to improve but may worsen their discomfort by taking the wrong medication for the wrong complication. Education enables individuals to match the pattern of their symptoms to the appropriate relief method rather than guessing.
Pain relief medications also require special attention in stomach care. While many people reach for over-the-counter painkillers to relieve stomach-related discomfort, not all pain relievers are safe for digestive problems. Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen are known to irritate the stomach lining and may worsen gastritis or contribute to ulcer formation. Taking NSAIDs on an empty stomach increases this risk further. In contrast, acetaminophen is usually gentler on the stomach and preferred for pain management in individuals with digestive sensitivity. These distinctions highlight why understanding the interaction between general medications and stomach function is just as important as knowing digestive-specific drugs. Pain relief should never be used to mask stomach complications without investigating their root cause; masking problems can delay diagnosis and allow conditions to progress.
As individuals learn about these medication categories and how they interact with the digestive system, they gain clarity on a fundamental medical reality: the stomach and intestines are sensitive organs that require balance. Medication should restore balance, not suppress messages from the body or replace healthy function. Many stomach complications improve significantly with lifestyle changes such as mindful eating, regular meals, reduced trigger foods, hydration, exercise, sleep regulation, and stress management. When medications are needed, they should be selected based on the specific physiological disturbance—not based on habit, assumption, or the experience of others. Because digestive systems vary from one person to another, a medication that relieves symptoms in one person may be ineffective or even aggravating in someone else. This reinforces the importance of professional consultation when symptoms are persistent, recurrent, severe, or accompanied by warning signs such as bleeding, weight loss, prolonged vomiting, fever, persistent diarrhea, or difficulty swallowing.
The most meaningful educational takeaway regarding stomach complication medication is the understanding that relief and healing depend on precision. Stomach acid problems require acid-focused treatment, infection requires anti-infective treatment, bowel irregularity requires motility-adjusting treatment, gas and indigestion require digestive support, and pain relief requires safe medication choices based on stomach sensitivity. Misuse occurs when medications are selected for the wrong underlying mechanism, taken too frequently, or used without addressing lifestyle causes. Proper understanding of digestive medication not only enhances symptom control but also protects long-term digestive function by preventing unnecessary dependence and avoiding complications.
Ultimately, education transforms medication from a quick fix into a supportive tool within a larger framework of digestive health management. When individuals recognize what each medication category truly does, respect the body’s signaling system, and apply medical guidance appropriately, they experience relief with confidence rather than uncertainty or trial-and-error self-treatment. This perspective empowers individuals to manage stomach complications wisely, respond early to concerning symptoms, and build a healthier lifelong relationship with their digestive system.