Human Kidney Chronic Disease — Renal Function Decline and Long-Term Organ Damage
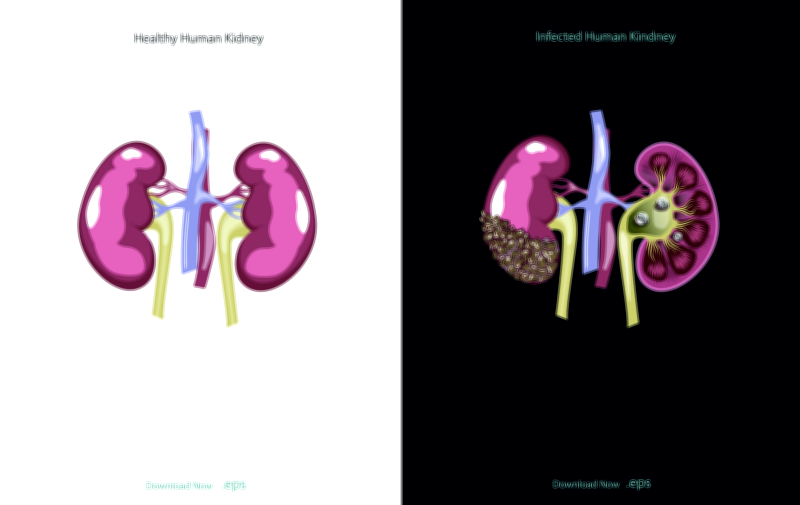
Chronic kidney disease is a progressive and long-lasting deterioration of kidney function that gradually reduces the organ’s ability to filter blood, regulate body fluids, maintain electrolyte balance, and eliminate metabolic wastes. The kidneys act as highly specialized biological filtration units, operating continuously to remove toxins, regulate blood pressure, maintain red blood cell production through hormone secretion, and stabilize the body’s acid–base equilibrium. In chronic kidney disease, these vital regulatory and excretory roles weaken slowly over months or years as kidney tissue becomes damaged. This gradual decline often goes unnoticed in early stages because symptoms remain mild or nonspecific while functional loss accumulates silently. Only when significant tissue damage has occurred do major disturbances in blood chemistry, fluid regulation, hormonal balance, and metabolic waste buildup begin to appear. Understanding chronic kidney disease involves exploring not just the anatomy and physiology of the kidneys themselves, but also the long-term effects of sustained injury, metabolic stress, inflammation, high blood pressure, diabetes, and lifestyle factors that progressively undermine renal capacity.
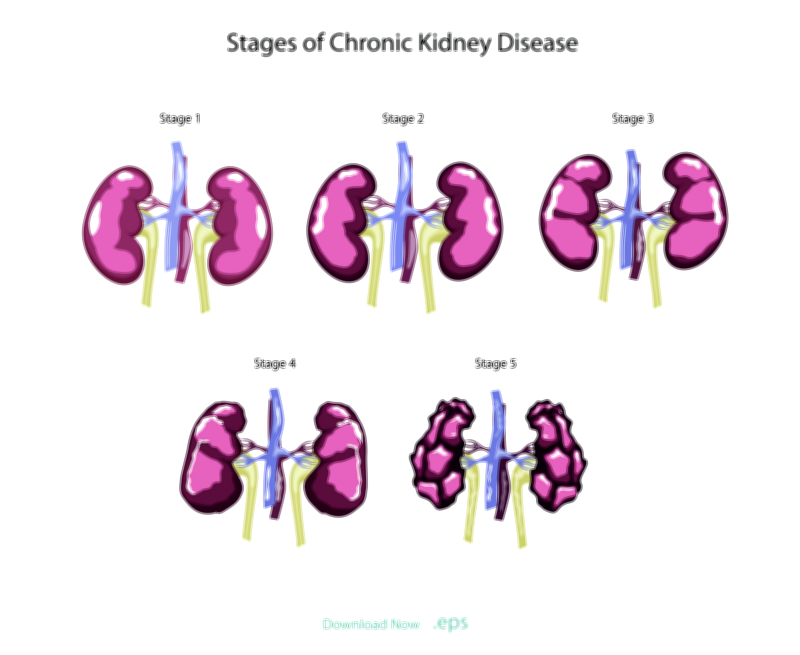
The structure of each kidney is composed of millions of tiny filtration units called nephrons, which perform the essential task of filtering blood plasma, separating wastes, retaining necessary nutrients and proteins, and modifying the final composition of urine. In chronic kidney disease, nephrons are damaged gradually. Once destroyed, they cannot regenerate, and the remaining nephrons begin working harder to compensate. This compensation is helpful initially, maintaining adequate function while the body continues daily tasks without noticeable change. However, the increased workload on remaining nephrons eventually becomes unsustainable, triggering a cascade of inflammation, scarring, and further nephron loss. The progression from mild kidney impairment to advanced chronic kidney disease therefore follows a vicious cycle in which damage promotes further damage. Over time, the kidney’s filtering surfaces shrink, scar tissue replaces functional cells, and the organ becomes smaller, denser, and less capable of performing its fundamental roles.
The early stages of chronic kidney disease are often physiological rather than symptomatic. Mild fluid imbalance, small changes in electrolyte levels, and slightly elevated blood urea or creatinine can appear in laboratory testing long before patients experience visible signs. This silent progression makes chronic kidney disease particularly dangerous because early treatment opportunities may be missed. As the disease advances into moderate stages, symptoms gradually emerge. Patients may experience swelling in legs or face due to fluid retention, chronic fatigue from anemia caused by reduced erythropoietin hormone production, muscle cramps, decreased appetite, nausea, and difficulty concentrating as waste products accumulate in the bloodstream. High blood pressure becomes both a cause and consequence of kidney damage because the kidneys regulate vascular volume and hormonal pathways that influence vascular resistance. As kidneys become compromised, blood pressure frequently rises, accelerating further tissue injury.
In severe or advanced stages of chronic kidney disease, the ability of the kidneys to maintain biochemical homeostasis becomes critically impaired. Fluid overload can cause congestive heart failure, pulmonary edema, and hypertension. Dangerous electrolyte imbalances—particularly high potassium—can disrupt heart rhythm and lead to life-threatening arrhythmias. Bone health deteriorates as failing kidneys lose their ability to regulate calcium and phosphorus metabolism, leading to bone weakening, fractures, and chronic pain. The entire body faces the toxic effects of waste retention, which can cause neurological complications such as confusion, sleep disturbances, or seizures. At the final stage—end-stage renal disease—the kidneys can no longer sustain life without replacement therapy. At this stage, dialysis or kidney transplantation becomes necessary to remove wastes and maintain fluid balance.
The causes of chronic kidney disease are diverse but share common pathways of injury to nephrons. Diabetes is the leading cause because chronically high blood sugar damages blood vessels within the kidney’s filtration units, promoting inflammation and scarring. High blood pressure follows closely because excessive vascular pressure damages delicate capillaries responsible for filtration. Autoimmune conditions such as lupus nephritis and IgA nephropathy trigger immune-mediated attacks on kidney tissues. Long-term use of certain pain medications, recurrent infections, congenital abnormalities, and inherited disorders like polycystic kidney disease can also lead to chronic damage. In many populations, lifestyle factors—including obesity, high-salt diets, smoking, excessive alcohol consumption, and lack of physical activity—contribute significantly to the gradual decline in renal function. These risk factors intertwine, making chronic kidney disease not just a medical disorder but a widespread public health issue that touches metabolic health, cardiovascular health, and socioeconomic conditions.
Management of chronic kidney disease centers around slowing disease progression, preserving remaining nephrons, and controlling systemic complications. Because damaged kidney tissue cannot be restored, treatment focuses on reducing workload and stress on the kidneys. Blood sugar control in diabetic patients, blood pressure management through medication and diet, reduction of dietary sodium, and careful regulation of dietary protein all help minimize metabolic strain. Medications that block the renin-angiotensin-aldosterone system play a central role because they lower intraglomerular pressure and reduce further filtration damage. Monitoring electrolytes, managing anemia, correcting bone mineral disorders with vitamin D analogs or phosphate binders, and controlling swelling with diuretics form key pillars of clinical care as the disease advances. Lifestyle improvements—such as smoking cessation, exercise, weight control, and hydration balance—also slow disease progression and improve cardiovascular health, which is a critical factor because cardiovascular disease is the leading cause of death among chronic kidney disease patients.
When kidney function falls below a critical threshold, replacement therapy becomes necessary to sustain life. Dialysis provides artificial clearance of metabolic wastes and fluid control through either hemodialysis performed using a vascular access route or peritoneal dialysis performed through the abdominal cavity. Although dialysis supports life, it cannot fully substitute for the hormonal and metabolic functions of the kidney, and it places major lifestyle restrictions on patients. Kidney transplantation, when available, offers the best long-term outcome, restoring more complete kidney function and providing greater quality of life. However, the need for lifelong immunosuppressants and the shortage of donor organs remain major challenges. Preventive care and early detection therefore remain the best strategies for reducing severity and improving outcomes.
Chronic kidney disease has deep emotional, psychological, and socioeconomic dimensions. Patients may face fatigue, anxiety, dietary restrictions, medication burden, dependence on dialysis therapy, and disruptions to employment or social life. Families often become involved in caregiving roles, and health systems face rising treatment costs as global rates of diabetes, hypertension, and metabolic disease continue to increase. Public health initiatives therefore emphasize routine screening for at-risk groups, patient education, early lifestyle interventions, and integration of kidney health into broader metabolic disease management frameworks.
At its core, chronic kidney disease is a long-term decline of renal function that reshapes nearly every major system of the body. It begins microscopically, progresses gradually, and culminates in widespread metabolic failure if untreated. Yet, early detection and lifestyle correction can slow and sometimes stabilize its progression, preserving quality of life and delaying or preventing the need for replacement therapy. By understanding both the biological mechanisms behind kidney damage and the systemic consequences of reduced renal function, patients and clinicians can work together to protect kidney health, prevent complications, and maintain long-term wellness.