Human Liver Disease — Progressive Organ Damage, Metabolic Imbalance, Immune Dysfunction, and Systemic Impact on Long-Term Health
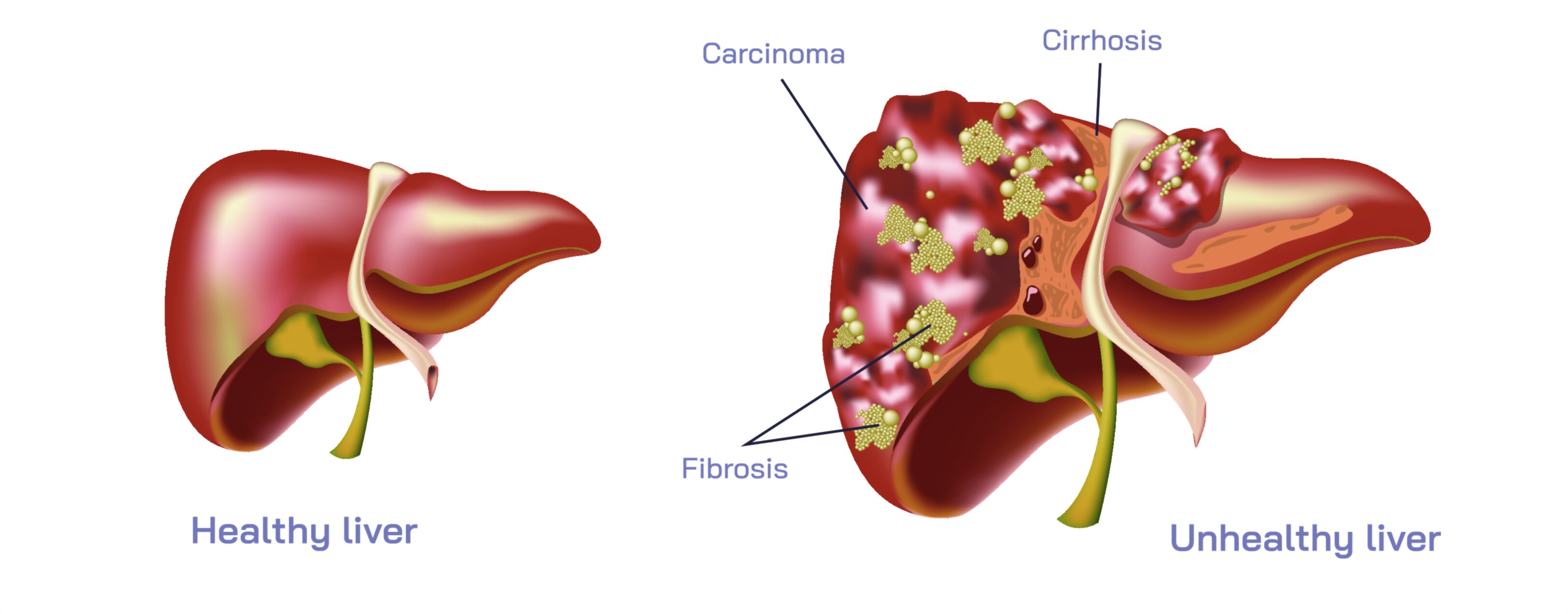
Human liver disease refers to any condition that disrupts the structure or function of the liver, an organ central to metabolism, detoxification, digestion, blood filtration, immune surveillance, and nutrient storage. Because the liver participates in nearly every major biochemical pathway in the body, diseases affecting it can lead to widespread systemic consequences. Liver disease is not a single entity but a large family of disorders that vary in cause, speed of progression, severity, and reversibility. Some forms of liver disease develop rapidly and dramatically within days, while others persist quietly for years before advancing to life-threatening stages. In nearly all cases, liver disease begins with injury to liver cells—whether from toxins, viruses, immune attack, fat accumulation, or genetic abnormalities—and leads to inflammation, tissue damage, and eventually scarring. The liver tries to heal, and when healing is incomplete, the substitute tissue becomes fibrosis, a rigid framework of scar tissue that gradually replaces functional liver cells. Over time, fibrosis may progress to cirrhosis, a condition in which the liver becomes hardened, nodular, and severely compromised. Whether driven by alcohol, metabolic disorders, viruses, autoimmune mechanisms, drug reactions, or inherited metabolic defects, human liver disease represents a slow but powerful unraveling of one of the body’s most vital biological engines.
Because the liver is involved in detoxifying chemicals, metabolizing medications, processing dietary nutrients, and filtering blood from the intestines, it faces constant metabolic pressure. When stressors accumulate faster than the organ can compensate, inflammation results. This early stage of injury is called hepatitis, meaning inflammation of the liver. Hepatitis can be temporary and reversible when the damaging trigger is removed, or it can become persistent if the trigger remains. Alcohol abuse is one of the oldest known causes of chronic hepatitis, as repeated heavy drinking disrupts fat metabolism, triggers oxidative stress, and promotes immune-based inflammation of liver tissue. In recent decades, metabolic dysfunction associated with obesity, insulin resistance, and sedentary lifestyles has accelerated the prevalence of fatty liver disease, a condition in which excess fat accumulates inside liver cells. What begins as simple fat deposition can evolve into inflammation and fibrosis if the metabolic imbalance persists. Viral hepatitis, particularly hepatitis B and hepatitis C, represents another major global cause, allowing chronic viral replication to attack liver cells continuously. Autoimmune liver disease emerges from the immune system mistakenly targeting the liver, while rare genetic disorders interfere with copper, iron, or enzyme metabolism, gradually poisoning the organ from within.
The early stages of liver disease are often silent. The liver has an extraordinary reserve capacity and can function adequately even when partially damaged. Many individuals feel completely well while their liver is already undergoing inflammation and fibrosis. This “silent phase” is one reason why liver disease frequently remains undiagnosed until scar tissue has accumulated. As fibrosis worsens and alters the structure of the organ, blood flow becomes restricted. Veins that should flow freely through the liver encounter resistance, raising pressure in the portal venous system that connects the intestines and spleen to the liver. With this mounting internal pressure come the first noticeable systemic changes. People may begin to experience fatigue, nausea, abdominal discomfort, bloating, swelling in the legs, itching, or jaundice—the yellowing of skin and eyes caused by bilirubin accumulation. Appetite and weight changes, bleeding tendencies, and increased vulnerability to infections can appear as liver function deteriorates. In progressive disease, the metabolic and detoxification roles of the liver begin to fail, leading to a chain reaction of problems affecting the brain, kidneys, digestive system, and cardiovascular system.
As scarring advances, cirrhosis develops. Cirrhosis is not merely “severe liver disease”—it is a structural collapse of the liver’s architecture. Normal soft, regenerative liver tissue is replaced by inflexible nodules of scar. The organ shrinks and hardens, losing both its mechanical flexibility and its ability to carry blood properly. With cirrhosis, portal hypertension becomes more pronounced, forcing blood to detour through fragile collateral veins in the esophagus, stomach, and abdomen, risking sudden and life-threatening ruptures known as variceal bleeding. Fluid accumulation in the abdomen (ascites) becomes common and may become infected, causing a dangerous complication known as spontaneous bacterial peritonitis. Because the liver normally filters toxins—especially ammonia—before they reach the brain, cirrhotic failure allows these toxins to circulate freely. When this happens, the brain becomes impaired, leading to headaches, memory problems, confusion, personality changes, sleep disturbances, and in severe cases, coma. This cluster of neurological symptoms is known as hepatic encephalopathy, one of the most devastating outcomes of liver failure.
Another major consequence of chronic liver disease is the heightened risk of hepatocellular carcinoma, the most common form of primary liver cancer. Unlike many cancers that arise spontaneously in healthy tissue, hepatocellular carcinoma often develops on the background of cirrhosis or chronic inflammation, where repeated cycles of cell death and regeneration create an unstable environment prone to genetic mutation. Because symptoms of liver cancer often overlap with those of cirrhosis, the diagnosis may occur late unless regular surveillance imaging is performed in high-risk individuals.
Diagnosis of liver disease involves evaluating both liver function and liver structure. Blood tests can reveal elevated enzymes released from damaged liver cells, reduced production of albumin and clotting factors, and abnormal bilirubin levels. Tests may also detect specific causes such as viral infection, autoimmune antibodies, or metabolic abnormalities. Imaging studies—ultrasound, CT scan, MRI and elastography—allow clinicians to visualize fat accumulation, fibrosis, blood-flow changes, nodules, and tumor development. In certain cases, a liver biopsy remains the most definitive method to assess the severity and pattern of damage, though newer non-invasive fibrosis assessments have reduced the need for biopsy in many patients. Early diagnosis dramatically improves outcomes, because interventions are most effective before extensive scar tissue forms.
Treatment of human liver disease varies according to its cause and stage. Removing the root trigger is the most powerful step: complete abstinence in alcohol-related liver disease, antiviral therapy for hepatitis B or C, treatment of metabolic dysfunction through weight loss and glucose control in fatty liver disease, immunosuppressive therapy in autoimmune hepatitis, or chelation in disorders of heavy metal accumulation. Supportive care focuses on managing complications, protecting remaining liver function, and maintaining adequate nutrition. As cirrhosis advances, specialized therapies may include medications to reduce portal pressure, diuretics for ascites, lactulose for encephalopathy, and endoscopic intervention for variceal bleeding. Once the liver becomes too damaged to sustain life, liver transplantation becomes the only definitive treatment option. Transplantation replaces the diseased organ with a healthy donor liver and can restore normal blood chemistry, metabolic function, and long-term survival if patients are eligible and immunologically managed after surgery.
Prevention remains critical because many types of liver disease are preventable or reversible in early stages. Reducing alcohol misuse, maintaining a healthy weight, eating a nutrient-rich diet, exercising regularly, avoiding unnecessary medications and toxins, and ensuring vaccination against hepatitis viruses significantly lower the risk of liver injury. Early screening for individuals at risk—especially those with obesity, diabetes, chronic alcohol exposure, or family history of liver disease—helps identify problems before irreversible damage occurs. Public-health efforts aimed at reducing viral hepatitis infection, improving food and water safety, and expanding access to medical care all reduce global liver disease burden.
Human liver disease ultimately reflects the tension between one of the body’s most resilient organs and the ongoing stresses it must endure across a lifetime. The liver can regenerate astonishingly—capable of re-growing tissue even after major surgical removal—but only when damaging influences are removed soon enough. Once fibrosis transforms into cirrhosis, the window for full recovery closes, and the focus turns to management rather than reversal. The future of liver disease treatment lies in continued advances in antiviral therapy, metabolic medicine, targeted immunology, fibrotic scar reversal, precision nutrition, and regenerative medicine. With deeper understanding of how liver injury evolves—and how the body attempts to heal itself—medicine moves closer to preventing organ failure before it becomes irreversible. In this way, human liver disease represents both a major global health challenge and an area of rapidly advancing scientific progress, where early awareness, timely intervention and ongoing medical support have the power to protect one of the body’s most essential organs and preserve long-term health.