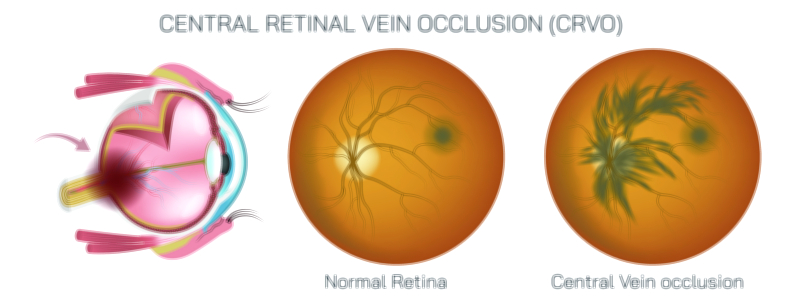
How a Normal Retina Differs From the Changes Seen in Diabetic Retinopathy
A normal retina functions as a finely organized visual layer, converting incoming light into signals that the brain interprets as clear images. Within this layer, tightly arranged cells gather information from the visual field and transfer it through delicate pathways toward deeper regions of the eye. Balanced support structures maintain steady nourishment, ensuring stable performance and continuous clarity. When this balance remains intact, the visual layer preserves fine detail and contrast across a wide range of lighting conditions.
In diabetic retinopathy, long term metabolic stress alters the fragile network that maintains this clarity. Small vessel walls may weaken, allowing fluid to escape into nearby regions. These subtle shifts can disturb the uniform arrangement of the visual layer, affecting how accurately signals travel toward deeper pathways. Over time, some areas may experience reduced nourishment, altering the consistency of the optical surface and influencing the overall quality of incoming detail.
As the condition progresses, additional changes may appear in regions responsible for fine detail processing. Fluid may accumulate, forming pockets that distort the smooth contour of the visual layer. These distortions disrupt how information spreads across central zones, reducing sharpness and making tasks such as reading or recognizing facial features more difficult. The surrounding structures may attempt to compensate, but alterations in distribution often limit the precision of these adjustments.
Understanding the contrast between a healthy visual layer and the altered patterns seen in diabetic retinopathy highlights the importance of metabolic stability for long term eye function. By observing how structural shifts influence clarity, researchers and clinicians gain insight into how early changes develop and how protective strategies can help preserve visual performance.