Collagen — Structural Protein of Connective Tissues
Collagen stands as one of the most abundant and essential proteins in the human body, forming the structural foundation for connective tissues that support, protect, and bind nearly every part of the body together. It is the biological glue that gives strength to bones, elasticity to skin, flexibility to cartilage, toughness to tendons, resilience to ligaments, and structural integrity to blood vessels, organs, and even the cornea of the eye. As a fibrous protein with a unique triple-helix structure, collagen is not just a passive material within tissues—it is actively produced, remodeled, repaired, and regulated to maintain the body’s mechanical stability and biological harmony. When we explore collagen deeply, we discover a remarkable protein that influences appearance, movement, healing, aging, and overall physical well-being. Its presence in virtually every connective system explains why collagen is central not only to cellular biology and medical science but also to nutrition, dermatology, orthopedics, and regenerative health.
At the molecular level, collagen is characterized by its tightly wound triple-helix structure, a configuration formed by three polypeptide chains intertwined like a strong rope. This triple helix provides extraordinary tensile strength, allowing tissues to resist stretching, tearing, and deformation. The composition of collagen is rich in amino acids like glycine, proline, and hydroxyproline, the latter of which requires vitamin C for its formation. This biochemical dependency explains why vitamin C deficiency leads to weakened collagen synthesis and the symptoms of scurvy—bleeding gums, fragile skin, joint pain, and poor wound healing. The body synthesizes collagen through a series of intricate cellular steps that take place primarily within fibroblasts, chondrocytes, and osteoblasts, depending on the tissue involved. After synthesis, collagen molecules self-assemble into fibrils and fibers that interweave with other proteins and extracellular matrix components, forming strong, flexible scaffolds that give tissues their form and function.
One of the notable characteristics of collagen is the existence of multiple types, each with distinct roles. More than twenty-eight types of collagen have been identified, but three types dominate human physiology. Type I collagen, the most abundant, is found in skin, bones, tendons, ligaments, and scar tissue. It provides tensile strength and rigidity, making it crucial for skeletal support, wound repair, and maintaining the firmness of the skin. Type II collagen is concentrated in cartilage, providing smooth, cushioning surfaces for joints and supporting the flexible structures of the respiratory tract. Degeneration of type II collagen contributes significantly to arthritis, joint stiffness, and mobility loss. Type III collagen supports the elasticity of organs, blood vessels, and the skin, often working alongside type I. It is also essential in early wound healing and tissue repair. Other specialized collagens serve functions in basement membranes, the eye, the placenta, and the filtration structures of the kidney. Together, these collagen types create a network of supportive architecture that allows the body to maintain resilience across a lifetime.
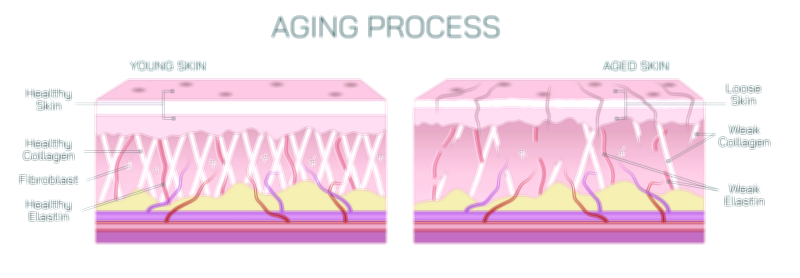
Collagen’s role becomes especially visible in the skin, where it forms major components of the dermis. Along with elastin and hyaluronic acid, collagen maintains the skin’s elasticity, density, hydration, and firmness. Over time, natural collagen production declines due to aging, sun exposure, environmental stress, hormonal changes, and lifestyle factors. As collagen fibers degrade and their replacement slows, the skin becomes thinner, less elastic, and more susceptible to wrinkling and sagging. This gradual decline marks one of the most visible signs of aging. Dermatology and cosmetic science focus heavily on understanding collagen dynamics to address skin aging. Treatments such as retinoids, vitamin C serums, microneedling, laser therapies, and peptide formulations aim to stimulate collagen production. When the dermal matrix is encouraged to rebuild, the skin becomes smoother, firmer, and more youthful in texture. Collagen’s importance in the skin underscores why it is central to the beauty and wellness industries, yet its scientific significance goes much deeper than appearance alone.
In the skeletal system, collagen contributes to bone structure by creating a flexible framework that mineral deposits—primarily calcium phosphate—adhere to. Without collagen, bones would be brittle and prone to fracture; with collagen, they become strong yet flexible enough to absorb impact. Conditions such as osteoporosis involve not only the loss of minerals but also changes in collagen quality, weakening the internal matrix that supports bone strength. Collagen is also the primary component of tendons, which anchor muscles to bones, and ligaments, which stabilize joints. These structures require exceptional tensile strength because they endure immense mechanical forces during movement. When collagen is healthy, joints remain stable, flexible, and resilient. When collagen becomes damaged through injury, aging, or degenerative conditions, mobility suffers, and pain or inflammation increases.
In cartilage, particularly the smooth cartilage that cushions joints, collagen works alongside proteoglycans and water to create a flexible, shock-absorbing tissue. Cartilage does not contain blood vessels, so its healing is slow and limited. Damage to cartilage, whether through injury or osteoarthritis, reflects a breakdown in collagen fibers that reduces the tissue’s ability to bear weight and cushion movement. Because cartilage regeneration is challenging, therapies often focus on supporting collagen formation or introducing regenerative techniques such as platelet-rich plasma (PRP) or stem cell therapy to stimulate fibroblasts and chondrocytes to rebuild collagen frameworks.
Collagen also plays key roles in the cardiovascular system. Type III collagen strengthens the walls of blood vessels and organs, ensuring elasticity and preventing ruptures. In conditions like aneurysms or vascular disease, collagen abnormalities may weaken vessel walls. Likewise, collagen’s presence in cardiac structures supports the rhythmic movement of the heart, contributing to the mechanical integrity needed for effective blood pumping. In the gastrointestinal system, collagen forms part of the connective tissues that support the intestinal lining, helping maintain barrier function and structural stability. Healthy collagen networks help prevent intestinal permeability, commonly referred to as “leaky gut,” and support digestive health.
The body constantly breaks down and rebuilds collagen through remodeling processes that adapt to physical demands, injuries, and metabolic changes. Collagen turnover is influenced by hormones (especially estrogen), dietary intake, genetic factors, oxidative stress, and overall health. Aging reduces the activity of fibroblasts, the cells responsible for producing new collagen. Environmental stressors such as ultraviolet radiation accelerate collagen breakdown by stimulating enzymes called matrix metalloproteinases (MMPs), which degrade collagen fibers. Smoking generates free radicals that damage collagen, impair oxygen supply, and slow tissue healing. Poor diet or inadequate protein intake deprives the body of the amino acids needed to synthesize collagen. These factors show that collagen health is strongly influenced by lifestyle choices and external exposures.
From a nutritional perspective, collagen requires specific building blocks to form properly. Amino acids derived from protein-rich foods support collagen synthesis. Vitamin C is essential for stabilizing the collagen triple helix, making fruits and vegetables critical for healthy connective tissues. Minerals such as zinc and copper assist in enzymatic processes that link collagen fibers together. Bone broth, fish skin, chicken cartilage, gelatin, and collagen supplements provide direct sources of amino acids that support collagen formation in the body. Although supplements do not send collagen directly to specific tissues, the peptides they contain supply the raw materials needed for cells to produce new collagen where it is required. Hydration also plays a role because water supports the extracellular matrix that collagen fibers inhabit.
Collagen’s role in wound healing is vital. When tissue is damaged, fibroblasts migrate to the wound site and begin producing collagen to rebuild structural integrity. Initially, type III collagen forms a softer framework, which is later replaced by stronger type I collagen as the wound matures. Scar tissue reflects this collagen-driven repair process, demonstrating how the protein restores strength even when the repaired tissue differs from the original.
Collagen disorders, whether genetic or acquired, highlight its central importance. Conditions such as osteogenesis imperfecta, Ehlers–Danlos syndrome, and certain connective tissue diseases arise from problems with collagen structure, synthesis, or cross-linking. These disorders cause extreme joint flexibility, fragile bones, skin fragility, vascular complications, and chronic pain. Their existence underscores how essential properly functioning collagen is for normal structural support.
Ultimately, collagen is far more than a structural component. It is a dynamic, adaptable, life-sustaining protein that reinforces tissues, supports movement, enables healing, maintains organ integrity, and shapes the appearance of the skin. Its presence throughout the body demonstrates the interconnected nature of human physiology—how microscopic molecular arrangements influence macroscopic structure and function. By understanding collagen’s roles, maintaining healthy lifestyle habits, and supporting its synthesis nutritionally and therapeutically, individuals can promote stronger tissues, more resilient joints, healthier aging, and improved overall well-being.