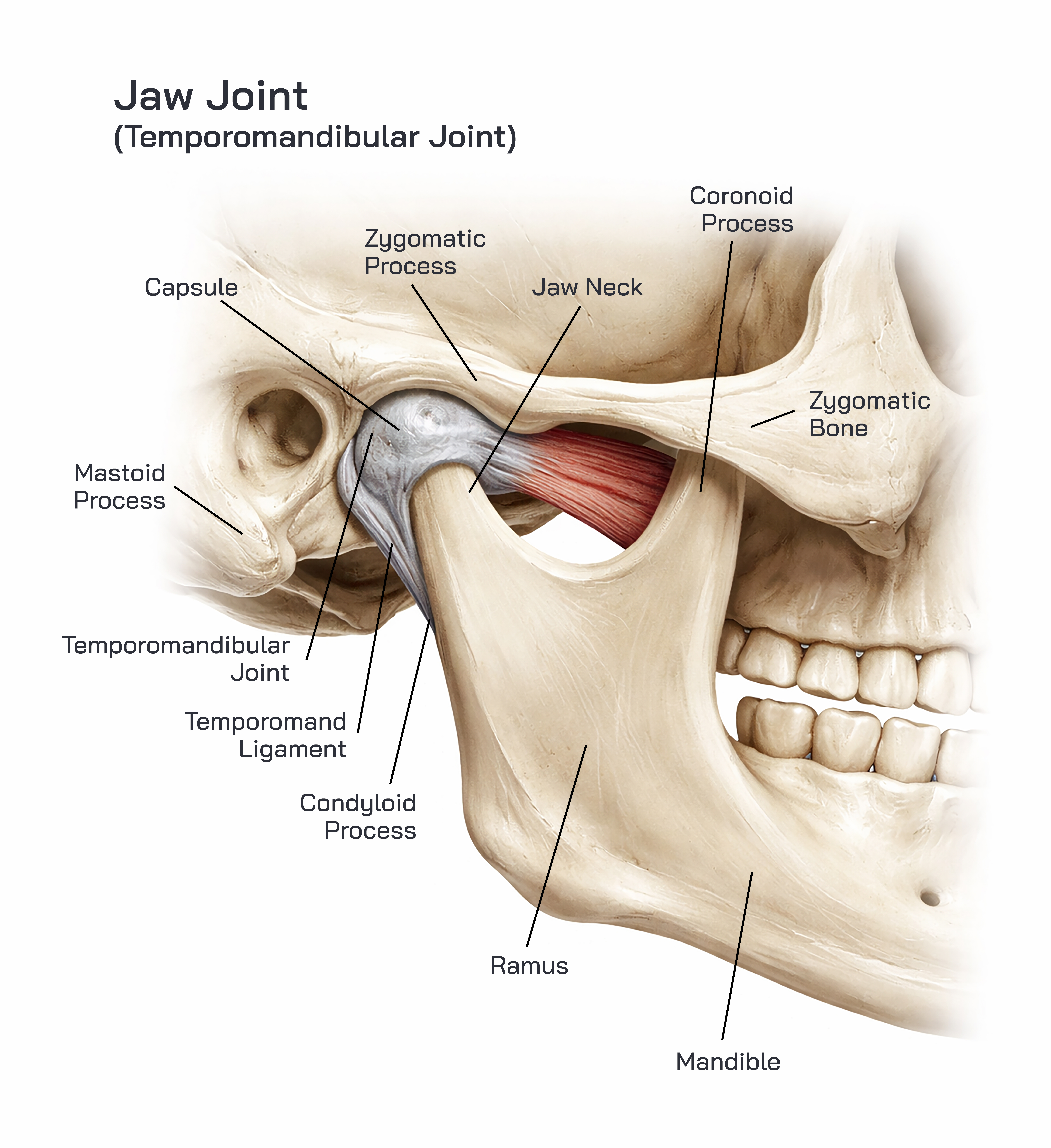
The temporomandibular joint, commonly known as the jaw joint, is one of the most complex and frequently used joints in the human body. It connects the lower jaw, called the mandible, to the temporal bone of the skull. This joint plays a vital role in everyday functions such as chewing, speaking, swallowing, yawning, and facial expression. Unlike many other joints that perform a single type of movement, the temporomandibular joint allows a combination of movements, making it uniquely adaptable and essential for normal oral function.
Anatomically, the temporomandibular joint is classified as a synovial joint, meaning it contains a joint capsule filled with lubricating fluid. However, it is functionally distinct because it combines both hinge and sliding actions. This dual function allows the jaw to move up and down as well as forward and backward. The ability to perform these complex movements enables precise control over biting, grinding, and speech articulation.
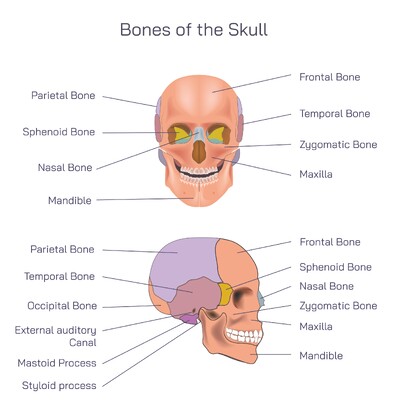
The primary bony components of the temporomandibular joint are the mandible and the temporal bone. The mandible forms the lower jaw and includes a rounded projection known as the mandibular condyle. This condyle fits into a shallow depression in the temporal bone called the mandibular fossa. Together, these structures form the main articulation of the jaw joint. The shape and alignment of these bones allow smooth movement while maintaining stability.
One of the most important parts of the temporomandibular joint is the articular disc. This disc is a strong yet flexible structure made of fibrous connective tissue. It sits between the mandibular condyle and the temporal bone, acting as a cushion that absorbs shock during jaw movement. The disc also helps distribute pressure evenly across the joint surfaces, preventing wear and damage. Its presence allows the jaw to move smoothly without direct bone-to-bone contact.
The joint capsule surrounds the temporomandibular joint and encloses all its internal components. This capsule helps maintain joint integrity and contains synovial fluid, which lubricates the joint surfaces. The synovial fluid reduces friction during movement and supplies nutrients to the articular structures. Proper lubrication is essential for smooth jaw function and long-term joint health.
Several ligaments support the temporomandibular joint and contribute to its stability. These ligaments limit excessive movement and prevent dislocation. They guide the jaw during opening and closing, ensuring that motion occurs within safe anatomical limits. The supportive role of ligaments is crucial, especially given the frequent and repetitive use of the jaw throughout the day.
Muscles play a central role in the function of the temporomandibular joint. These muscles control jaw movement and provide the force needed for chewing and speaking. Coordinated muscle activity allows the jaw to open, close, move forward, and shift side to side. This muscular control ensures precise movement and balance between strength and flexibility. Without proper muscle coordination, normal jaw function would be compromised.
Functionally, the temporomandibular joint allows two main types of movement. The first is rotational movement, which occurs when the jaw opens and closes like a hinge. This movement happens primarily in the lower compartment of the joint. The second is translational movement, where the mandible slides forward and backward. This sliding motion occurs in the upper compartment and is essential for wide mouth opening and grinding actions during chewing.
Chewing, also known as mastication, is one of the primary functions of the temporomandibular joint. During chewing, the joint allows coordinated movements that break down food into smaller pieces for digestion. The combination of hinge and sliding motions enables efficient grinding of food, increasing the surface area for digestive enzymes. This function is critical for proper nutrition and digestive health.
Speech is another important function supported by the temporomandibular joint. Precise jaw movements help shape sounds and control articulation. Even subtle movements of the jaw contribute to clarity and expression in speech. The joint’s flexibility and control allow rapid adjustments in jaw position, supporting fluent communication.
Swallowing also depends on proper temporomandibular joint function. The jaw must open and close smoothly to position food correctly in the mouth. Coordinated movement between the jaw, tongue, and throat ensures safe and efficient swallowing. Any disruption in joint function can interfere with this process.
The temporomandibular joint also contributes to facial balance and alignment. Proper jaw positioning supports even distribution of forces across the teeth and facial bones. This alignment helps maintain dental health and prevents excessive stress on individual structures. Balanced joint function is essential for maintaining a comfortable bite and overall oral stability.
From a biomechanical perspective, the temporomandibular joint is designed to handle repeated use and significant force. Chewing generates strong pressure, yet the joint’s structure allows it to absorb and distribute this force effectively. The articular disc, synovial fluid, ligaments, and muscles all work together to protect the joint from damage.
Clinically, understanding the parts and functions of the temporomandibular joint is essential in dentistry, medicine, and physical therapy. Jaw joint issues can affect chewing efficiency, speech clarity, and overall quality of life. Knowledge of normal joint anatomy helps in identifying abnormal movement patterns and maintaining joint health.
The temporomandibular joint represents a remarkable example of biological engineering, uniquely adapted to perform a wide range of precise, repetitive, and forceful movements while maintaining stability and comfort. What sets this joint apart from most others in the human body is not only its complexity, but also the degree to which it must coordinate with teeth, muscles, nerves, and posture to function properly. Every bite, word, and facial expression depends on this joint operating in a finely balanced manner.
One of the most unique aspects of the temporomandibular joint is that it functions as a paired joint. The left and right joints must work together in perfect coordination, even though they are anatomically separate. When the jaw moves, both joints respond simultaneously, adjusting position and force distribution. This bilateral dependency means that dysfunction on one side often affects the other, highlighting how delicately balanced jaw mechanics are. Few other joints in the body are so interdependent in daily function.
Another distinctive feature is the joint’s relationship with the teeth and bite alignment. The way the upper and lower teeth meet directly influences how the temporomandibular joint moves and bears load. Proper alignment allows forces to be distributed evenly through the joint and surrounding muscles. Even small changes in tooth position or bite pattern can alter joint mechanics, increasing stress on specific structures. This close connection explains why dental health and jaw joint health are deeply linked.
The articular disc within the temporomandibular joint deserves special attention for its adaptive role. Unlike cartilage found in many other joints, this disc is composed of dense fibrous tissue, making it more resistant to wear and compression. Its shape is carefully contoured to match the condyle and temporal bone, allowing it to move dynamically as the jaw opens and closes. Rather than remaining stationary, the disc shifts position to maintain optimal contact and cushioning throughout different jaw movements.
The joint compartments above and below the articular disc perform different mechanical roles. The lower compartment primarily facilitates rotational movement, allowing the initial opening and closing of the mouth. The upper compartment supports translational movement, enabling the jaw to glide forward and downward during wider opening. This division of labor allows the jaw to achieve a greater range of motion than a simple hinge joint could provide, while still maintaining control and stability.
Muscle coordination around the temporomandibular joint is exceptionally refined. Multiple muscles work together in carefully timed sequences to produce smooth movement. Some muscles generate power for biting and chewing, while others guide fine positioning and stabilization. During complex actions like chewing, muscles on one side may contract while others relax, allowing side-to-side motion. This intricate coordination allows for efficient food processing and precise control during speech.
The nervous system plays a critical role in temporomandibular joint function. Sensory receptors within the joint, muscles, and surrounding tissues continuously provide feedback to the brain about jaw position, tension, and movement. This sensory information allows for rapid adjustments, preventing excessive force or awkward positioning. Such feedback is essential for protecting the joint during activities that require strong biting forces or rapid movement changes.
Posture also has a significant influence on temporomandibular joint mechanics. Head and neck alignment affect the resting position of the jaw and the tension in jaw muscles. Poor posture can subtly alter joint loading patterns over time, increasing strain on certain structures. This connection explains why jaw discomfort is sometimes associated with neck or upper back issues, even when the joint itself appears structurally normal.
The temporomandibular joint is designed to withstand constant use. Unlike joints such as the knee or shoulder, which experience periods of rest, the jaw joint is active throughout the day. Chewing, swallowing, speaking, and even unconscious movements during sleep place demands on the joint. Despite this constant activity, the joint is remarkably durable when properly balanced and supported by healthy muscles and alignment.
Adaptability is another defining characteristic of the temporomandibular joint. The joint can adjust gradually to changes in bite, tooth wear, or muscle use. This adaptability helps maintain function over time but also means that gradual imbalances may go unnoticed until symptoms develop. The joint’s ability to compensate can mask underlying issues, making early awareness and preventive care important.
From a developmental perspective, the temporomandibular joint continues to mature through childhood and adolescence. Jaw growth, tooth eruption, and muscle development must remain coordinated for optimal function. Disruptions during these stages can influence joint mechanics later in life. This developmental aspect underscores the importance of monitoring jaw alignment and function early on.
In daily life, the temporomandibular joint contributes not only to basic survival functions but also to social interaction. Facial expressions, speech nuances, and emotional communication all rely on subtle jaw movements. The joint’s flexibility allows humans to express a wide range of emotions through facial cues, reinforcing its role beyond simple mechanical function.
From a biomechanical standpoint, the temporomandibular joint manages both compressive and shear forces. Chewing generates vertical pressure, while sliding movements introduce horizontal forces. The joint’s structure, including the articular disc and synovial fluid, distributes these forces efficiently, reducing stress on any single component. This ability to manage complex force patterns is a hallmark of its design.
Clinically, the temporomandibular joint serves as a reminder that function is as important as structure. A joint may appear anatomically normal yet function poorly if muscle coordination, posture, or bite alignment is disrupted. Conversely, minor structural variations may cause no issues if functional balance is maintained. This perspective emphasizes the importance of viewing the jaw joint as part of an integrated system rather than an isolated structure.
The temporomandibular joint is not only one of the most complex joints in the human body, but also one of the most finely regulated. Its uniqueness lies in the fact that it must function continuously with extreme precision while tolerating significant mechanical loads. Unlike joints that primarily support posture or locomotion, the jaw joint is responsible for tasks that demand both strength and delicacy, often within the same moment. This dual requirement has shaped a joint system that is anatomically sophisticated and functionally adaptable.
A defining feature of the temporomandibular joint is its integration into a larger functional chain. The joint does not act alone; it operates as part of a coordinated system involving the teeth, facial bones, muscles of mastication, cervical spine, and nervous system. Any change in one component can influence the behavior of the joint as a whole. This interconnectedness explains why jaw function is sensitive to seemingly unrelated factors such as posture, stress levels, or dental alignment.
The joint’s ability to glide as well as hinge is essential for efficient oral function. When the mouth opens slightly, the movement is mostly rotational, occurring within the lower joint compartment. As the mouth opens wider, the condyle and disc shift forward together, allowing increased opening without strain. This smooth transition between movement types prevents excessive pressure on the joint surfaces and enables wide mouth opening without instability. Few joints in the body demonstrate this kind of seamless movement transition.
Another remarkable characteristic is how the temporomandibular joint distributes force asymmetrically during chewing. Chewing rarely occurs on both sides simultaneously. Instead, one side often bears more load while the other stabilizes or guides movement. The joint structures are designed to handle this uneven force distribution repeatedly without damage. This requires precise disc positioning, muscle coordination, and ligament control to prevent excessive wear.
The articular disc itself is a dynamic structure rather than a passive cushion. It adapts its position continuously in response to jaw movement. During chewing, the disc shifts slightly to maintain optimal contact between the condyle and temporal bone. This adaptability protects the joint surfaces and reduces friction. The disc’s fibrous composition allows it to resist compression while remaining flexible enough to move with the joint.
The temporomandibular joint is also unique in its sensory richness. It contains numerous mechanoreceptors that detect pressure, movement, and joint position. These receptors provide constant feedback to the brain, allowing fine-tuned control of jaw movements. This sensory input is crucial during activities like speech, where small adjustments in jaw position can significantly affect sound production. Without this feedback system, precise oral function would not be possible.
The influence of emotional and psychological states on the temporomandibular joint is another distinctive aspect. Stress and emotional tension often manifest physically through increased jaw muscle activity. Clenching or grinding the teeth, especially during sleep, places additional strain on the joint and surrounding structures. This mind–body connection highlights how the temporomandibular joint responds not only to mechanical demands but also to neurological and emotional signals.
From an evolutionary perspective, the temporomandibular joint reflects adaptation to complex dietary and communicative needs. As human diets diversified and speech became more refined, the jaw joint evolved to support varied movements beyond simple biting. The ability to grind food efficiently and articulate complex sounds required a joint capable of precise, controlled motion rather than brute force alone.
The joint’s relationship with the cervical spine further emphasizes its systemic role. Head and neck alignment influence jaw position at rest and during movement. Forward head posture can shift the resting position of the mandible, altering joint loading patterns. Over time, this can increase strain on specific joint components. This relationship underscores the importance of viewing jaw health in the context of overall musculoskeletal balance.
Adaptation is one of the temporomandibular joint’s strengths, but it can also be a weakness. The joint often compensates for imbalances in bite or muscle function, maintaining usability despite underlying issues. While this adaptability allows continued function, it can delay the onset of noticeable symptoms. By the time discomfort or dysfunction appears, compensatory patterns may already be well established.
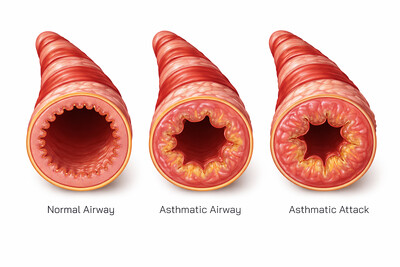
The temporomandibular joint also plays a subtle role in breathing and airway function. Jaw position influences tongue placement and airway space, particularly during sleep. Proper joint alignment supports open airway posture, while altered positioning can contribute to airway narrowing. This connection illustrates how jaw mechanics can influence systems beyond chewing and speech.
Another unique aspect is the joint’s exposure to repetitive microtrauma. Chewing, speaking, and swallowing occur thousands of times per day. Each movement applies small forces that accumulate over time. The joint’s resilience depends on balanced muscle activity, adequate lubrication, and healthy disc positioning. When these factors are maintained, the joint tolerates lifelong use remarkably well.
Developmentally, the temporomandibular joint reflects growth patterns of the entire facial skeleton. Changes during childhood and adolescence influence jaw alignment and joint mechanics in adulthood. Proper development requires coordination between bone growth, tooth eruption, and muscle function. Disruption during these stages can influence joint behavior later in life, highlighting the importance of early monitoring.
In social interaction, the temporomandibular joint supports nonverbal communication. Smiling, frowning, and subtle facial movements depend on jaw stability and mobility. These expressions play a crucial role in human interaction, reinforcing the joint’s importance beyond basic survival functions.
In summary, the temporomandibular joint is a highly specialized structure designed for continuous, precise, and adaptable movement. Its paired coordination, dynamic articular disc, rich sensory feedback, and integration with posture, emotion, and breathing make it unlike any other joint in the body. Rather than functioning in isolation, it operates as part of a complex system that reflects the interconnected nature of human anatomy. Understanding this joint in depth reveals how seemingly simple actions like chewing or speaking rely on an extraordinary level of biological coordination and balance. The temporomandibular joint is one of the most sophisticated joints in the human body. Its paired nature, adaptive articular disc, precise muscle coordination, sensory feedback, and close relationship with teeth and posture make it uniquely capable of handling complex demands. Every aspect of its anatomy is designed to support both power and precision, allowing humans to eat, speak, and express themselves with remarkable efficiency. Understanding this joint in depth reveals not only its mechanical brilliance, but also its essential role in daily life and overall well-being.
In conclusion, the temporomandibular joint is a highly specialized and multifunctional joint that supports essential daily activities. Its parts include the mandible, temporal bone, articular disc, joint capsule, ligaments, and muscles, all working together to enable smooth and controlled jaw movement. The functions of the jaw joint extend beyond chewing to include speech, swallowing, and facial coordination. Understanding the structure and function of the temporomandibular joint highlights its importance in oral health, communication, and overall human physiology.