Heel pain is one of the most common yet most difficult foot conditions to manage because it interferes with both movement and weight-bearing activities. When the heel becomes painful, daily routines such as standing, walking, climbing stairs, and exercising suddenly require extra effort and can even become unbearable. Among the numerous causes of heel discomfort, two stand out as frequent triggers: stress or overload involving the phalanges and inflammation of the plantar fascia, more commonly known as plantar fasciitis. Although these issues affect different structures of the foot, they are closely connected because the heel, the plantar fascia, and the phalanges work together during every step. When one component becomes strained, the entire biomechanical chain begins to break down.
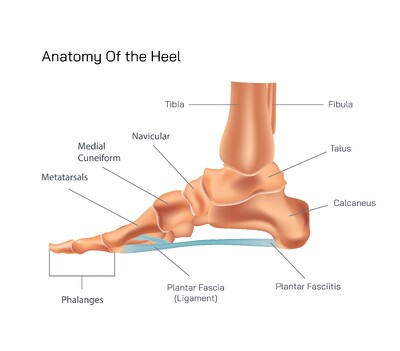
The phalanges—better known as the toe bones—play a crucial role in the propulsion phase of the gait cycle. They stabilize the foot, grip the ground, and assist in distributing pressure when pushing off during walking or running. When excessive stress is repeatedly placed on the toes due to poor footwear, improper running mechanics, tight calf muscles, high-impact sports, or long hours of standing, the phalanges become overloaded and transmit excessive tension back to the heel. This overload disrupts the designed balance of pressure distribution and leads to irritation of the tissues that anchor the heel to the rest of the foot.
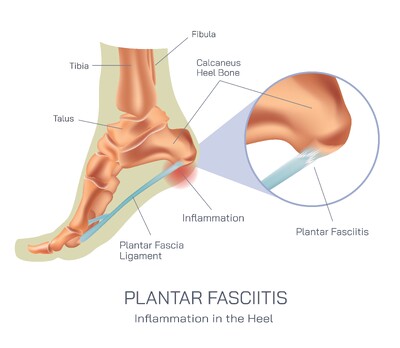
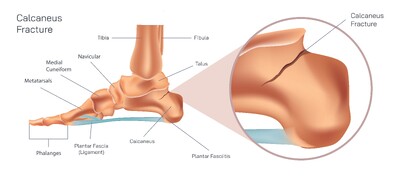
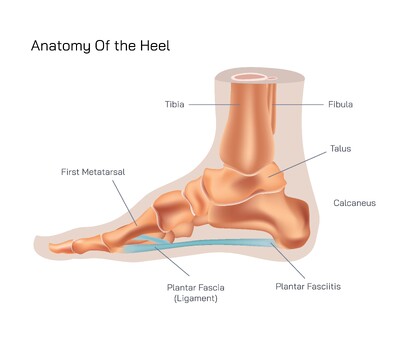
The plantar fascia, a long thick band of connective tissue stretching from the calcaneus to the base of the phalanges, becomes the primary victim of this mechanical imbalance. It is responsible for maintaining the arch of the foot and absorbing shock during every step. When tension increases beyond its tolerance, microscopic tears develop within the fascia, causing inflammation and sharp pain around the heel. This condition, known as plantar fasciitis, is widely recognized by its characteristic symptom of intense pain when first stepping out of bed in the morning or after long periods of rest. The pain often improves slightly after movement begins but returns with extended activity as tissues become fatigued again.
The heel becomes a central point of pain not because it is weak, but because it is a biological force transfer center. Every step begins with heel strike, proceeds through the midfoot, and ends with push-off from the toes. When the phalanges are stressed or the plantar fascia is strained, the heel absorbs increasing mechanical overload, eventually causing persistent pain. Foot structure also influences heel discomfort. Individuals with flat feet experience excessive stretching of the fascia, while people with high arches often place excessive downward force onto the heel pad. Tightness of the Achilles tendon further increases tension on the heel by restricting ankle flexibility and applying constant downward pull on the calcaneus.
Heel pain affects not only the foot itself but also the body’s posture and movement patterns. To avoid discomfort, many individuals unconsciously adjust their gait, shifting weight to the forefoot or outside edge of the foot. Over time this compensation can lead to knee discomfort, hip misalignment, and even lower back pain. People with untreated plantar fasciitis or phalangeal overload may gradually lose mobility, avoid physical activity, and experience diminished quality of life due to constant fear of triggering pain.
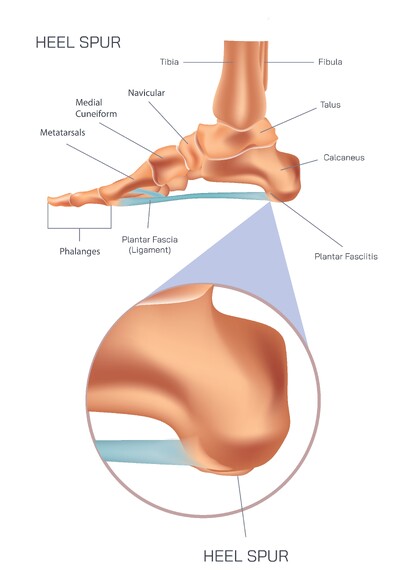
Diagnosis of heel pain requires careful examination of symptoms, foot alignment, pressure distribution, and activity patterns. Clinicians may perform palpation to identify sensitivity around the plantar fascia or phalanges and evaluate tendon tightness. Ultrasound may reveal thickened fascia, while X-rays are useful when bone spurs or fractures are suspected. Monitoring how pain fluctuates throughout the day — particularly morning pain and post-activity flare-ups — is also an important indicator of plantar fascia involvement.
Treatment focuses on reducing inflammation, restoring tissue elasticity, and correcting mechanical overload. Stretching programs targeting the calf muscles and Achilles tendon relieve excessive pull on the plantar fascia. Gentle strengthening of intrinsic foot muscles supports the arch and reduces strain on the heel. Footwear modification is one of the fastest ways to reduce symptoms — cushioned soles, soft heel counters, and supportive midsoles reduce irritation during walking. Orthotic inserts provide additional arch stability and help realign pressure distribution away from the heel. Ice therapy following activity remains an effective tool for short-term relief.
For persistent symptoms, targeted medical interventions may be considered. Shockwave therapy stimulates tissue repair and reduces chronic inflammation in resistant cases. Platelet-rich plasma injections aim to accelerate healing of microscopic tears. In extreme or long-standing cases where conservative methods fail, surgical treatment may be considered to release tension in the fascia or address structural abnormalities affecting pressure distribution. Fortunately, most patients recover without surgery when management is consistent and holistic.
Preventing the recurrence of heel pain requires lifelong awareness of biomechanics and foot care habits. Proper warm-up before exercise, avoiding sudden increases in training intensity, wearing shoes designed for specific activities, and maintaining flexibility in the calf muscles protect the heel from strain. Alternating high-impact exercises with low-impact activities like swimming or cycling can give the heel periodic relief without sacrificing fitness. For individuals whose work involves prolonged standing, cushioned insoles and short periodic stretching breaks make a meaningful impact.
Heel pain caused by phalangeal overload and plantar fasciitis is not a condition that appears overnight, and it cannot be resolved overnight. It is a gradual process of mechanical stress that requires a gradual approach to healing. The most successful recovery occurs when treatment relieves inflammation, restores tissue flexibility, and improves the body’s overall movement mechanics instead of focusing solely on pain control. With consistent care, most individuals regain comfort, mobility, and confidence in their physical activity, leaving heel pain behind and restoring an active lifestyle without fear of every step.