Tooth Decay — Stages, Causes, and Prevention Explained
Tooth decay is one of the most common chronic health problems worldwide, affecting people of all ages and developing so gradually that serious damage often occurs long before pain becomes noticeable. At its core, tooth decay is a biological process in which acids produced by harmful bacteria dissolve tooth minerals faster than the body can repair them. This imbalance progresses through predictable stages, beginning with microscopic demineralization and potentially ending in deep infection, tooth loss, and systemic health complications if untreated. Although many people associate tooth decay only with “cavities,” the condition actually reflects a broader chain of events driven by diet, oral hygiene habits, saliva composition, and bacterial behavior. Understanding the entire decay pathway—from early enamel weakening to advanced structural destruction—reveals how preventable tooth decay really is, and why intervention must focus not only on treatment but on interrupting the biological cycle that fuels it.
The decay process begins in the earliest stage: enamel demineralization, where the hard outer surface of the tooth loses minerals due to recurring acid exposure. The enamel, although the strongest substance in the body, is not immune to chemical erosion. After every sugary or carbohydrate-rich meal, bacteria in dental plaque metabolize sugars and produce acids. If these acid attacks occur frequently, minerals such as calcium and phosphate begin to dissolve out of the enamel. At first, this stage appears only as faint white chalky spots indicating weakened enamel. There is no pain, no hole, and no visible loss of tooth structure, which is why many individuals are unaware that decay has already started. The crucial aspect of this stage is that it is fully reversible. With proper oral hygiene, fluoride exposure, and mineral replenishment, the enamel can rebuild and return to strength without permanent damage. However, if the acid environment continues, the demineralization becomes deeper and progresses into later stages.
As decay advances, the process enters the enamel decay stage, where surface breakdown becomes permanent. Minerals are lost faster than they can be replaced, leading to small defects that enlarge over time. A cavity begins to form—a literal hole in the surface—but pain is still unlikely because enamel contains no nerves. At this point, the opportunity for natural reversal has passed; the only way to stop progression is through professional treatment to remove damaged tissue and seal the area with restorative materials. Ignoring decay at this stage creates a pathway for bacteria to invade deeper layers of the tooth, eventually making the problem more painful and difficult to control.
If decay is not treated during enamel breakdown, it reaches the dentin decay stage, where damage becomes significantly worse. Beneath the enamel lies dentin, a softer, more porous layer that surrounds the tooth’s nerve (pulp). Dentin dissolves far more easily than enamel, so once decay reaches this layer, it spreads rapidly. At this stage, sensitivity begins to appear—especially to sweets, cold drinks, or brushing—because dentin contains microscopic tubules connected to the pulp. Chewing may also become uncomfortable. The presence of bacteria inside dentin triggers inflammation in the pulp chamber, increasing pressure inside the tooth. Without urgent treatment, the decay progresses even faster.
The next stage, pulp infection, marks the point when decay penetrates the inner core of the tooth. The pulp contains nerves and blood vessels that keep the tooth alive. As bacteria invade the pulp, inflammation becomes intense and pressure builds inside a rigid structure that has no room to expand. This causes severe, persistent toothache that may radiate into the jaw, ear, or head. Pain may worsen at night or when lying down because of increased blood flow to the head. At this point, the infection is no longer confined to the tooth surface—bacteria now live inside living tissue. Without intervention such as root canal therapy to remove infected pulp and disinfect the tooth, the infection continues to spread.
When the pulp infection advances beyond the tooth, it reaches the abscess stage, one of the most serious phases of dental disease. Pus accumulates at the root tip, forming a pocket of infection that can spread into gums, jawbone, and surrounding tissues. Swelling, fever, bad taste in the mouth, and severe throbbing pain are common signs. If untreated, the infection can spread into the bloodstream or airways, becoming a systemic medical emergency. At this stage, saving the tooth becomes increasingly difficult and tooth extraction may be the only safe option. The contrast between this stage and the early reversible stage illustrates how tooth decay is not one event but a progressive pathway that becomes increasingly aggressive with every step.
Deciphering how decay develops requires understanding its underlying causes, which form a chain reaction rather than a single trigger. The process begins with plaque buildup, a sticky layer of bacteria that forms constantly on teeth. When plaque is not removed through brushing and flossing, it thickens and becomes a stable environment for acid-producing bacteria. Diet plays a major role: sugary foods, snacks, carbonated beverages, candies, and frequent grazing feed bacteria and accelerate acid production. What matters more than the total amount of sugar is frequency of exposure. Snacking all day keeps the mouth in a continuous acid state, giving enamel no time to recover. Additionally, saliva quality affects decay risk. Healthy saliva neutralizes acids and supplies minerals to rebuild enamel, but dry mouth—caused by dehydration, certain medications, or mouth breathing—greatly increases decay risk. Lifestyle habits such as heavy alcohol consumption, smoking, and poor oral hygiene intensify bacterial growth and weaken enamel. Some individuals also have deeper grooves, crowding, or genetic enamel differences that make cleaning more difficult, increasing susceptibility. Tooth decay therefore does not occur randomly; it follows predictable biological logic based on the balance between bacterial acids and enamel resistance.
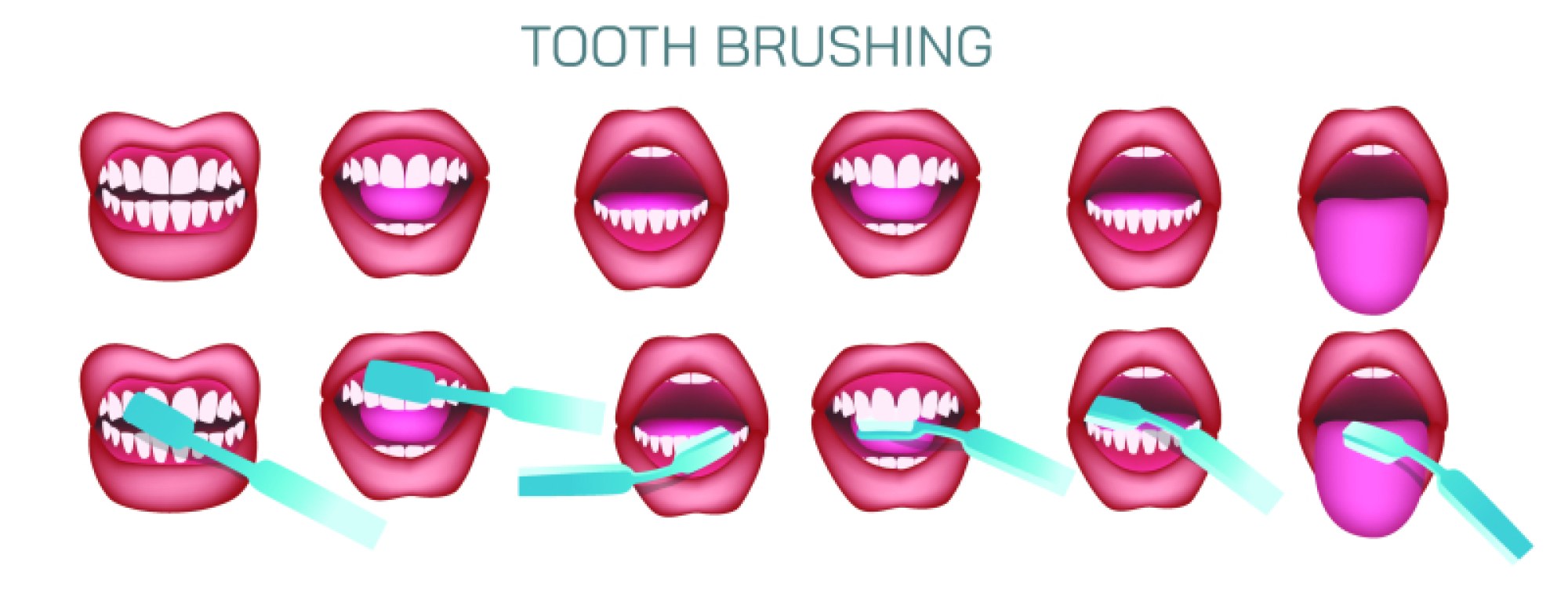
Fortunately, the same biological logic also provides a roadmap for prevention, built around interrupting or reversing the decay cycle. Daily brushing with fluoride toothpaste and thorough flossing remove plaque and prevent harmful bacteria from colonizing tooth surfaces. Fluoride plays a crucial role because it integrates into enamel crystals to make them more acid-resistant and stimulates remineralization. Diet modifications can dramatically reduce decay risk: limiting frequent snacking, reducing sugary and acidic drinks, choosing water between meals, and eating fiber-rich foods that stimulate saliva naturally. Dental check-ups and professional cleanings remove tartar—hardened plaque that cannot be removed at home and serves as a bacterial reservoir. Protective treatments such as fluoride varnish or dental sealants strengthen enamel and cover deep grooves where bacteria hide. Even small daily habits—rinsing after meals, drinking enough water, chewing sugar-free gum to stimulate saliva—contribute to creating a mouth environment that prevents decay progression.
The contrast between the earliest and the most advanced stages of decay demonstrates that prevention is not simply an oral hygiene recommendation—it is a strategy that protects both dental and overall health. Early decay is painless and reversible, while late decay is painful and sometimes irreversible. Recognizing subtle signs early—chalky white patches, sensitivity to cold or sweets, bad breath, or staining—can preserve tooth structure and avoid extensive procedures. When prevention fails, dentistry shifts from preservation to reconstruction, requiring fillings, root canals, or extractions depending on the stage of damage.
Tooth decay, therefore, should not be viewed as a sudden event but as a progressive interaction between bacteria, diet, saliva, hygiene, and time. Its prevention depends not on eliminating bacteria completely—that is impossible—but on controlling their environment and supporting natural enamel repair processes. When we understand the stages of decay, we appreciate the immense value of early action and healthy habits. And when we view prevention as the first treatment, we preserve not only the appearance of a bright smile but the biological integrity of teeth that are meant to last a lifetime.